[From the archives; originally posted October 20, 2005]
Measles is one of those diseases that we don't give much thought to in the United States anymore. Following an incubation period of about 10 days, flu-like symptoms appear: fever, malaise, cough, congestion, conjunctivitis. Soon, the rash appears, first near the ears, then the forehead, the face, and over the rest of the body. Complications were common. These could include a seconary bacterial pneumonia, encephalitis, myocarditis, miscarriage, and a condition called subacute sclerosing panencephalitis (SSPE).
(Continued below...)
SSPE is a progressive, generally fatal, brain disorder caused by chronic measles virus infection. It follows ~7-10 years after measles virus infection, and generally kills within 3 years from the onset of symptoms. And it's a nasty way to go: the patient suffers from behavioral changes, cognitive deterioration, vision problems, and eventually, advanced neurologic symptoms such as severe spasms, and finally, severe physical and mental impairment that leads to death. Risk factors for developing SSPE including contracting the measles virus at an early age (especially before age 2). Males also are more commonly affected than females. When the first live attenuated measles vaccine was licensed here in 1963, approximately 8 million deaths per year worldwide were the result of measles infection (or complications thereof), and ~50 cases of SSPE were reported each year in the U.S. Following vaccination, the numbers of SSPE cases have dropped dramatically; we now see only 1 or 2 cases per year, and those are almost always in patients who come from countries where measles is more of a problem than in the U.S. By any measure, the introduction of measles vaccination in the U.S. was successful at controlling the disease.
But success often breeds complacency. In the 1980s, rates of measles vaccination decreased, particularly among children less than 5 years of age, and those living in poverty. Anyone who's familiar with public health knows what comes next--an outbreak of measles infections. Indeed, an epidemic of measles occurred during 1989-1991: 55,622 measles cases and 123 measles-associated deaths were reported. From JID 189:S1:
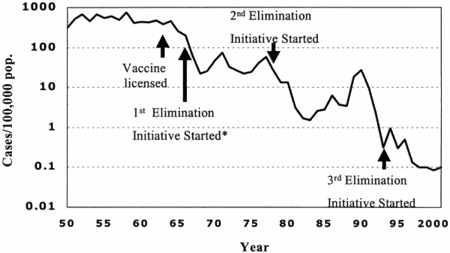
A problem with the measles vaccine--and with many vaccines--is that one dose may not be enough to prevent an infection with the natural virus. Therefore, many children who did not receive booster shots of the vaccine were incompletely protected; several developed measles during the 1989-91 outbreak. Some parents blamed this on the measles vaccine, which also has been linked to other conditions, such as autism (more on that here). A current Journal of Infectious Diseases study (JID 192:1686-93) used brain tissue and measles virus typing to determine whether the measles vaccine strain or natural measles virus infection was responsible for these cases of SSPE.
To do this, they took brain tissue from 11 patients diagnosed with SSPE, performed reverse-transcriptase PCR (necessary because measles is an RNA virus), and analyzed the sequences of the PCR products in order to determine the genotype of the measles virus. (Measles has 22 known genotypes; the vaccine strain, for example, is genotype A). None of the sequences matched the genotype A viruses--the vaccine was not causing SSPE.
However, based on their data, they do suggest that the risk of SSPE from measles was underestimated using older data. Using estimates of measles virus infection in the 1960s and 70s, a 1982 paper suggested that SSPE occurred in ~8.5 cases/million measles virus infections. Estimates from the current JID paper put it at closer to 6.5-11 cases of SSPE per 100,000 cases of measles--7-13 times higher than the earlier estimates.
What does all this mean, and why does it matter?
 In 1999, measles still caused 873,000 deaths per year, and accounts for almost half of the 1.6 million vaccine-preventable deaths in children every year. The Red Cross and associated agencies began a campaign in 2000 to reduce this number, akin to the polio and smallpox eradication efforts. They concentrated on sub-Saharan Africa, where 95% of the measles deaths worldwide occurred. By 2003, deaths were already down by 39% (to just over 500,000 in that year). Still, 500,000 vaccine-preventable deaths every year is way too many. And resistance to this vaccination remains, and by some accounts, is growing, in the United States. People forget that these "benign childhood diseases" can, and do, kill, and that vaccines are a public health intervention that has saved many millions of lives around the world.
In 1999, measles still caused 873,000 deaths per year, and accounts for almost half of the 1.6 million vaccine-preventable deaths in children every year. The Red Cross and associated agencies began a campaign in 2000 to reduce this number, akin to the polio and smallpox eradication efforts. They concentrated on sub-Saharan Africa, where 95% of the measles deaths worldwide occurred. By 2003, deaths were already down by 39% (to just over 500,000 in that year). Still, 500,000 vaccine-preventable deaths every year is way too many. And resistance to this vaccination remains, and by some accounts, is growing, in the United States. People forget that these "benign childhood diseases" can, and do, kill, and that vaccines are a public health intervention that has saved many millions of lives around the world.
The eradication of smallpox due to vaccination was a public health milestone. We no longer have endemic polio or measles in the United States, and global elimination of those diseases has been discussed. But this only works if everyone plays their part, and doesn't allow the small risk of side-effects outweigh the large benefit of vaccination.
- Log in to post comments

Tara -
Might I respectfully request that you reword the following sentence for clarity?
As you are of course aware, the review in the URI provided states that a link between the MMR vaccine and autism was proposed, but that the bulk of the evidence does not support the hypothesis that a link exists. A casual reader might take "has been linked to ... autism" as an endorsement of the MMR -> autism hypothesis.
Overall, an excellent post. I was not a regular reader when it came out the first time, so I'm glad you brought it back. Keep 'em coming!
Shock horror!
- we are currently seeing an upswing in measles infection in the UK. Notheing to do with our crappy papers feeding the public with crappy stories from crappy doctors trying to make money on the back of an unproven hypothesis that the MMR vaccinne causes autism.
no it has to be someone elses fault...???
http://badscience.net/forum/viewtopic.php?t=134
http://badscience.net/forum/viewtopic.php?t=133
or in fact chenck any link to MMR on 'badscience'
http://badscience.net
at least the dodgy doctor that is the cause of all this misery id up before the British medical council (GMC):
http://news.bbc.co.uk/1/hi/health/5070670.stm