 As I described previously in this post, war and disease are inextricably intertwined:
As I described previously in this post, war and disease are inextricably intertwined:
War and its concomitant devastation and social upheaval leaves its victims at an increased risk of disease transmission to begin with due to poor sanitation, collapse of public health and medical facilities and support personnel, crowding in refugee camps, breaks in supply chains of food, medicine, and other necessary items, malnutrition and depression, and other factors.
This social upheaval frequently lasts much longer than the actual fighting. Additionally, in some cases where areas have been destabilized from decades of conflict, any semblance of public health infrastucture is long gone, worsening the severity and duration of outbreaks of infectious disease.
Such is the case currently in Angola. I'd singled out this country previously as a war-torn area, with respect to an outbreak of Marburg virus:
Following independence from Portugal, Angola has suffered through 30 years of civil war. Estimates suggest that 1.5 million have been killed, and up to 4 million displaced during this time, and the population has been generally left in poor health with any public health infrastructure decimated.
The country is bereft of doctors, and the conditions make it difficult for international agencies to work there. This kept the 2005 Marburg epidemic, which killed 227 people, off the international radar for at least 6 months after it began, and it's also played a role in fueling the ongoing cholera outbreak there. More after the jump.
Vibrio cholerae is a water-borne bacterium that can cause severe intestinal infections. These can be so dehydrating that they may lead to death, after the elimination of copious amounts of "rice-water stools." Though once a scourge in the United States (an 1848 outbreak killed 4,000 people in New York City alone), cholera is mainly a disease of developing countries today, where poor sanitation and unclean drinking water facilitate spread and transmission of the bacterium.
I briefly mentioned the Angola cholera outbreak back in June. At that point, over 1,200 people had died, and 34,000 had been sickened in the outbreak, which began around February of 2006. Tthe lion's share of cases came from the capital city of Luanda, which was heavy with refugees displaced from decades of warfare. Many of the city's inhabitants lived in shanties without sanitation and clean water, so it's not surprising a water-borne epidemic was able to take hold there.
Currently, the number of cases and deaths have approximately doubled from what I noted in June--estimates stand at more than 2,700 deaths and 69,000 cases to date, almost a year into the epidemic. Additionally, it's spreading: all but one of the country's provinces have been affected. And worse, there is no end in sight. International agencies such as UNICEF have been working to distribute both clean fresh water and chlorine tablets to disinfect water where clean water can't be brought, to the at-risk population, but that population continues to grow and swamp the volunteers. Volunteers have also gone door-to-door distributing soap and bleach, and teaching people how to protect themselves and their family as best they can, but these are all stop-gap measures. What is really needed is a centralized source of clean drinking water and modern sewage systems to keep fecal matter from contaminating said drinking water, thereby continuing to spread cholera throughout the population. This can be done relatively cheaply when you consider a cost-benefit analysis (especially compared to other expenditures), but it's still an enormous output of money and time.
UNICEF has more on the magnitude of the water problem in Angola:
According to UNICEF and WHO, 50 per cent of Angolans do not have access to safe water, and only 30 per cent are using adequate sanitation facilities. Because of 27 years of war here, millions of displaced people live in deplorable conditions in overcrowded slums.
"The cholera outbreak in Angola is a painful reminder of the threat facing more than 1 billion people who have no access to clean water sources worldwide," says UNICEF Senior Programme Officer Akhil Iyer. "And, as is the case far too often, it's the young who suffer most."
I've mentioned the extent of this problem (lack of access to fresh water and general sanitation) previoiusly here. Though I've given talks on global health issues to the med students each semester I've been here, the magnitude of the problem still overwhelms me (and generally, completely shocks the medical students):
An estimated 1.1 billion persons (one sixth of the world's population) lack access to clean water and 2.6 billion to adequate sanitation.
Cholera is not difficult to control, as the reduction in disease in Victorian Europe and the United States demonstrated. Clean water and adequate sanitation typically stop an outbreak in its tracks, but when so much of the world's population lacks even these basic necessities, cholera will continue to re-appear, and many of the world's most vulnerable will suffer from it. These outbreaks, unfortunately, can last years, and the current one in Angola shows no sign of stopping any time in the immediate future.
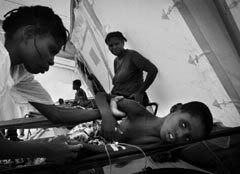
Image from http://www.artsenzondergrenzen.nl/usermedia/angola_cholera.jpg
- Log in to post comments

Very informative and scary post, Tara. I keep wondering how much we have overloaded our water treatment facilities in the developed countries as well. How long before we start seeing similar problems right in our own backyard? Global warming is a long distance problem timewise, safe drinking water is a today problem.