 I mentioned in the Introduction to Microbiology and Infectious Disease that many people don't understand the difference between a commensal and a pathogenic organism. I also mentioned that I'd try to write something about microbial ecology. Since I just gave a lecture yesterday on normal human flora in health and disease, now seems as good a time as any to combine these two and discuss just what it means when microbiologists refer to "normal flora" or "commensal organisms," and to talk about the microbial ecology of the human body in a series of posts on this topic.
I mentioned in the Introduction to Microbiology and Infectious Disease that many people don't understand the difference between a commensal and a pathogenic organism. I also mentioned that I'd try to write something about microbial ecology. Since I just gave a lecture yesterday on normal human flora in health and disease, now seems as good a time as any to combine these two and discuss just what it means when microbiologists refer to "normal flora" or "commensal organisms," and to talk about the microbial ecology of the human body in a series of posts on this topic.
First, though, a short note on terminology, as there are a number of other terms that are, essentially, interchangable. Sometimes you'll see our normal flora referred to as "commensal" microbes, meaning that they may derive benefit from us but typically don't cause us harm. In the literature, you'll also come across the more science-y term "indigenous microbiota," or perhaps "microbiome," to refer to the same collection of organisms. I'm going to use "normal flora" throughout this series, just because it's a personal preference. And so, without further ado, Part I begins after the jump...
What are "normal flora," and what do they do?
Though microbes tend to get a bad rap as causes of disease, the vast, vast majority of them are harmless. Indeed, an enormous amount of them live amongst us: these are your "normal flora". By the numbers, our body is more bacterial than human by a factor of about ten to one. They live in every possible niche on and within our bodies: on our skin; in our mouth, nose, and throat; in our gastrointestinal tract; in our genitourinary tract; in our conjunctiva. They are with us from the moment we are born to the moment we die, typically causing us no ill effects. Indeed, they benefit us in many ways. Arguably most important, they fill niches that would otherwise be available to pathogens we may be exposed to. Due to the presence of our normal flora, invading pathogens may find it more difficult to establish colonization and begin an active infection. This can be due to a number of factors. First, these bacteria simply take up space that could otherwise be exploited by an invading pathogenic species. Second, normal flora can locally exhaust micronutrients that pathogenic (disease-causing) bacteria need for metabolism, thereby inhibiting the growth of these invaders if they do enter the body. Third, byproducts produced by these normal flora can also make the local environment inhospitable for some species of pathogenic bacteria. (These byproducts can include chemicals such as acids or hydrogen peroxide that have general antimicrobial properties, or compounds such as antibiotics that kill organisms more selectively).
These normal flora rarely cause disease in the host. However, it does happen on occasion. Particularly in women, for example, bacteria from the rectum may be inadvertently moved from the perineal area to the urethra, with the result potentially being a urinary tract infection. Additionally, the presence of skin abrasions and cuts that allow normal flora to cross the epithelial cell barrier, or a condition which causes the host to be immunocompromised , can result in disease caused by the normal flora. However, these are relatively rare events, and typically our normal flora do much more good than harm to our bodies.
Normal flora versus "pathogenic" bacteria--how do we distinguish between them?
A problem arises, though, when what may be "normal flora" to one individual is a cause of severe disease in others. Many of us are colonized with organisms that would more typically be classified as "pathogens"--in other words, species which are generally associated with disease. These can include various disease-causing strains of E. coli in the intestinal microflora, or Streptococcus pyogenes in the throat, or Staphylococcus aureus in the nasal cavity. Though these may not cause any symptoms of disease in the host (therefore, they are part of their "normal flora"), they can still be transmitted to others and make them ill. Therefore, for species such as these, the line between "commensal" organism and "pathogen" is not clear-cut. (I'll discuss this further in a later post on different "strains" of microbes; stay tuned).
Difficulties of studying "normal flora"
As I mentioned, species which commonly are pathogenic represent only a very tiny fraction of all bacteria. However, what we know about these relatively few species represents the bulk of all scientific knowledge about bacteria. Therefore, we know little to nothing about the vast majority of bacteria which make up our normal flora--and when I say "vast majority," I'm not referring to a trivial number here. For example, it's estimated that there are approximately 400 different species of bacteria in the human oral cavity, and only ~150 of those have been cultured. We see a similar ratio when we examine normal flora in other areas of our body as well--there's just a lot of collective ignorance about so many of the species that inhabit us, for a variety of reasons.
A main reason for this ignorance is the fact that many of the species that make up our commensal organisms have never been cultured in a lab. This is typically our first step toward understanding an organism: isolate it from a complex mixture, grow it on a nutrient media in a "pure culture" (that is, separate from the other organisms that reside in said complex mixture), and do experiments on it--for example, to learn about its metabolism, or antibiotic resistance, or evolutionary history, etc. We have none of this information for most of the species that we're in contact with every day, not only in and on our own bodies, but in the larger environment as well. In the next post, I'll discuss other ways that we can study these microbes, independent of culture.
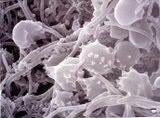
Image from http://www.bact.wisc.edu/themicrobialworld/dental_plaque.jpg
- Log in to post comments

Hmmm...I wonder if there have been studies done to illumninate the risk factors associated with using TP versus using a bidet (or both) for instance?
Thanks for the enlightening posts Tara.
"By the numbers, our body is more bacterial than human by a factor of about ten to one"
Tara, when you say this, do you mean bacterial organisms relative to human cells? You can't mean mass (or I'm going to be having nightmares).
Jake--right, by cell number.
Aw, shucks, and here I thought I'd be able to lose a huge amount of weight by just taking some broad-spectrum antibiotics...
Nifty post! Is there much hard science research on "probiotics" (like "live and active cultures" yogurt and such)? I know I've seen a few very focussed studies ("Effects of Lactobacillus somethingorotherus strain ZXKUQYB27 ingestion on fecal pH" and suchlike) but I've not gotten around to looking for broader studies.
(Still waiting for "Natural Flora Skin Lotion" and "Natural Flora Mouthwash"...)
Nice post.
The NY times has a blurb on a PNAS paper describing the diversity of bacteria on the forearms of six individuals.
link
It is striking (but maybe not surprising) that at least on the skin the turnover appears to be high. I am going to have to look at the paper. I wonder how variable the skin community is from place to place on the body of one individual.
SMC, I'll likely touch on probiotics in the third post I'm planning on this, discussing normal flora and health/disease.
Andrew, thanks for the story--that will fit in well here this week!
I believe the proper term for probiotics is Lactobacillus gimmickus ;-)
Thanks, Tara. Wow, fascinating. I had no idea our commensals helped us by simply filling literal niches within us, but given the pressure on all organisms to evolve and use all resources available, it certainly makes sense.
Hi, I was just wondering..most of the normal flora seem to bacteria..is it possible for any virsuses to present as normal flora ? or perhaps some moulds ?
Yep, both. I'm going to concentrate on bacteria for a few reasons--1) that's what I know best, and 2) that's what's been most studied (even in this fairly meager field), but certainly some species of fungus and many viruses inhabit us and cause us no harm, and even potentially are beneficial.
"the vast, vast majority of them are harmless. Indeed, an enormous amount of them live amongst us:"
I think you could go farther to say that we really could not live without these symbioses. That is, they are not just 'harmless' but are vital to our survival. Not only do they protect against pathogens but perform many functions that enhance our nutrition, etc. And there is probably much more, as we are largely ignorant of these relations.
Hi,
I have looked for "iron" on your site and found close to nothing. As you certainly will know a very basal defense mechanism is to increase ferritin intracellularly to bind iron and reduce its availability to invaders. This works because most pathogens (except many viruses) need iron for multiplication and activity (including plasmodium...: give children with malaria - which as a result become (more) anemic - iron and "help" plasmodium kill those children...; cf. ED Weinberg's review on the role of iron in infection and cancer as early as 1984 in Physiol Rev).
Ask your students to explain the very different smell of feces of a breast-fed baby and an adult man. (Lacotoferrin is a very important term not found on your site...)
Once you appreciate those very basic mechanisms you can easily explain e.g. why so many more men get ulcer disease (in non-cardia gastric cancer the difference in risk is "only" about factor 2) - H.pylori needs iron, of course. You also can explain why evolution has resulted in vaginal epithelium "feeding" lactobacilli with glycogen, while "upstream" lactoferrin is secreted into the cervical mucus.
You even can explain why regular blood donors smell better than people with ample "surplus" iron in their bodies. And you might ask yourself (and others) why in the US all flour has been supplemented with iron for more than half a century: In Denmark this "murderous" habit was stopped in the eighties, in Sweden in the nineties - but US gov. "experts" do seem to know better... (Obviously they don't realize that by far the most common inherited disorder is the predisposition to store iron, with all kinds of molecular mechanisms involved, not only loss-of function mutations in the Hfe-282-gene, widely propagated for commercial reasons.)
Front-line victims are for example Pima indians in Arizona, especially male Pima, who have a very high risk of type2 diabetes and complications, reducing their average life expectancy by some 15 years, compared to the US average (which is several years shorter than in comparable countries, cf. Francesco S. Facchini, "The Iron Factor of Aging: Why Do Americans Age Faster?" 2002). This has little to do with infection but is central to the etiology of age-related diseases in affluent societies.
Other prominent writers on iron and disease are Jerome L. Sullivan (VA/USA), J.T. Salonen (Kuopio/Finland) and former Harvard medical chemist Randall B. Lauffer, to name just a few. It's so very easy to stay healthy by getting rid of "surplus" iron - and it has been known for milleniae as a very effective therapy for "red" hypertension in ageing men, for example.
Wikipedia is definitely wrong in broadly stating: "Today it is well-established that bloodletting is not effective for most diseases, or at best less effective than modern treatments." Cf. Tuomainen et al. on the dramatic reduction in MI risk in male Finnish blood donors (BMJ 314, 1997), or on the absolutely terrific effect of iron depletion on about a dozen risk factors by serial phlebotomies in older Californians with insulin resistance/type2 diabetes (until a slight decrease in hematocrit), published in 2002 by F.S. Facchini & K.L. Saylor in the Ann NY Acad Sci Vol. 967.
There even is a disease where you can SEE the iron (hemosiderin..) in the skin "at work", that is varicose/venous leg ulcer(ation)... I HOPE that it will take less than ten years until Sullivan, Salonen and perhaps Facchini will receive the Noble Prize. This might speed etiology knowledge more than hundreds or even thousands of clinical and lab studies and papers on the role of iron in disease.
Etiology research (mainly by data mining) has been my top interest for more than a dozen years at Tuebingen/Germany: I could write a book on ignored infectious causes alone (e.g. MS/borreliosis; RA/P.mirabilis UTI, cf. Alan Ebringer, King's College/London, and MUCH more)... Perhaps you could include these topics in coming posts, and eventually we might succeed in stimulating interest in real progress in medicine, that is in primary prevention (cf. Pasteur, R.Koch etc. more than a century ago), not in ever more complex and expensive therapies.
I admit that I don't know much about what excess iron can do, but I do know that diptheria is caused by iron deficiency.
"...compounds such as antibiotics that kill organisms more selectively."
Surely, Tara, you realize that not all antibiotics "kill organisms more selectively." In fact, broad-spectrum antibiotics, which kill almost indiscriminately, are becoming increasingly popular by prescribers since doctors are not willing to take the time necessary to properly identify pathogenic bacteria and broad-spectrum agents are more likely to resolve the acute symptoms. Yet, they are also much more likely to disturb the balance of natural flora in the body. Therefore, your wording from the above is misleading.
Otherwise, a good post.
Kevin
Please read in context--more selectively than chemicals found in typical cleaners, such as peroxide, or vinegar, or bleach, etc. Obviously I realize there is a wide variety of specificity among antibiotics.
Please read in context...Obviously I realize there is a wide variety of specificity among antibiotics.
Tara, you have to first provide the appropriate context before your readers can "read in context." Your original statement was misleading and speaks to your sycophant tendencies. Let me explain. Your idea of writing "carefully" appears to mean that you must be careful not write anything that will reflect poorly on the current scientific consensus. Why else would fail to realize that the appropriate context was never provided for understanding the misleading phrase, "kill organisms more selectively".
However, the greater negligence is illustrated by the following: antibiotic resistance, though important, is the politically correct concern and you've no doubt mastered the party line, but a discussion of the other big concern, the negative effects of broad-spectrum antibiotics on human flora, is sadly underserved by your article. Perhaps, you'll have an opinion on the matter when your peers tell you what to think.
I think I'll rescind my "good article" compliment.
Kevin
Kevin,
First, please notice this series is incomplete, and this post is certainly not meant to be comprehensive alone. I mentioned at the end of part 2 that the next installment will focus more on normal flora and health, including what happens with disruption of normal flora (not only due to antibiotics, but due to invading microbes as well). Regular readers also know that I've discussed several times on this blog the importance of overall bacterial ecology in health and disease.
Second, I wasn't discussing manmade antibiotics in the part you pulled out. The surrounding text is:
(emphasis mine) I'm talking in that snippet of products produced by *our own normal flora*, not exogenous antibiotics taken for medicinal purposes. I'm sure you know that many of our antibiotics are microbial in origin, and these are being produced all the time by our normal flora and our own bodies (note this post on peptide antibiotics all of us produce, for example.)
Nice post.thanks..
nice working thanks. ;)
www.r10.net küresel ısınmaya hayır seo yarıÅması
Tara, really, you should take some time to consider things the other way around.
Not
A person is ill because of certain bacteria
but
A person is ill and therefore there are certain bacteria
Cut out the REsearch every once in a while and do a search in new places, you'll be surprised. Google "Antoine Bechamp", go and have a thourough look. NOW
Well, maybe you shouldn't. Where would you blog about Antoine Bechamp and the like? People would start to call you names and all that. No, maybe you'd better stick to the fancy places, it can be quite incomfortable to be a denialist, you know.
Thanks
http://www.geyikblog.com
Thanks for your post!
thanks
http://htmlkodlari.bloggum.com
Hi
how can I distingwish between pathogenic and normal flora in a culture medium ?
with best wishes to you thank you .
thanks for all
what specific diseases does normal flora protect us from?