 One of the most famous stories in all of epidemiology revolves around the very birth of the science, in the midst of a London cholera outbreak in 1854. At the time, the scientific community was divided over the cause of cholera and other diseases. The majority of them accepted the miasma theory, the idea that disease was due to corrupted air ("all smell is disease," noted sanitation commissioner Edwin Chadwick). This idea dates back to antiquity, and increased in popularity in the Victorian era. It's a great example of something that logically made sense, even though it was wrong. 19th century sanitation reformers pointed out to disease outbreaks that occurred in areas that were filthy, and along with that filth came a terrible smell. It was thought that the scent was due to the putrefaction of the air, and that when this putrid air was inhaled, it resulted in the development of disease. Again, it made sense--when areas were cleaned up, disease frequently decreased--it seemed like a no-brainer. Though this was prior to the formulation of the germ theory of disease, some scientists (dubbed "contagionists") believed disease was not acquired via miasma, but instead passed from person to person via some sort of unidentified particle.
One of the most famous stories in all of epidemiology revolves around the very birth of the science, in the midst of a London cholera outbreak in 1854. At the time, the scientific community was divided over the cause of cholera and other diseases. The majority of them accepted the miasma theory, the idea that disease was due to corrupted air ("all smell is disease," noted sanitation commissioner Edwin Chadwick). This idea dates back to antiquity, and increased in popularity in the Victorian era. It's a great example of something that logically made sense, even though it was wrong. 19th century sanitation reformers pointed out to disease outbreaks that occurred in areas that were filthy, and along with that filth came a terrible smell. It was thought that the scent was due to the putrefaction of the air, and that when this putrid air was inhaled, it resulted in the development of disease. Again, it made sense--when areas were cleaned up, disease frequently decreased--it seemed like a no-brainer. Though this was prior to the formulation of the germ theory of disease, some scientists (dubbed "contagionists") believed disease was not acquired via miasma, but instead passed from person to person via some sort of unidentified particle.
Physician John Snow was one of the early supporters of the latter theory. His careful investigation of the 1854 London cholera outbreak was the beginning of the end of the miasma theory--and the beginning of modern epidemiology as well. However, the impact of the cholera epidemic extends much farther than just the eventual formulation of the germ theory of disease and the downfall of the miasma theory. In The Ghost Map, Steven Johnson tells the fascinating history of John Snow's groundbreaking investigation, and how it still reverberates in the world today.
The Ghost Map is mostly a story of the cholera investigation, and especially John Snow's role in it. At the time, Snow was already a noted physician, famous for his studies on ether and chloroform anaesthesia. He carefully determined dosages of these chemicals that could be used in surgery and during childbirth, and was so successful that Queen Victoria even had him attend to the birth of her son. However, Snow wasn't content to limit himself to one area of study. Instead, he published research in a wide variety of areas--writing about lead poisoning, smallpox, scarlet fever, and the circulatory system, among others. He also long held a fascination with cholera, first discussing that topic in a pair of manuscripts in 1849. These documented a cholera outbreak that began the previous year, and left 50,000 dead by the time it ended. In these papers, Snow advanced his theory about the cholera's cause and transmission, suggesting 1) that the disease was transmitted by water, not air; and 2) that it was due to some as-yet-unidentified agent present in the water. So yes, cholera was a disease of filth, but it was due to dirty water, not fetid air.
Not surprisingly, Snow encountered much disagreement with his ideas. He knew that, while his work was solid and it showed a convincing correlation between water and cholera, he'd not proved causation. What he needed was, as a newspaper suggested, an experimentum crucis:
The experimentum crucis would be, that the water conveyed to a distant locality, where cholera had been hitherto unknown, produced the disease in all who used it, while those who did not use it, escaped.
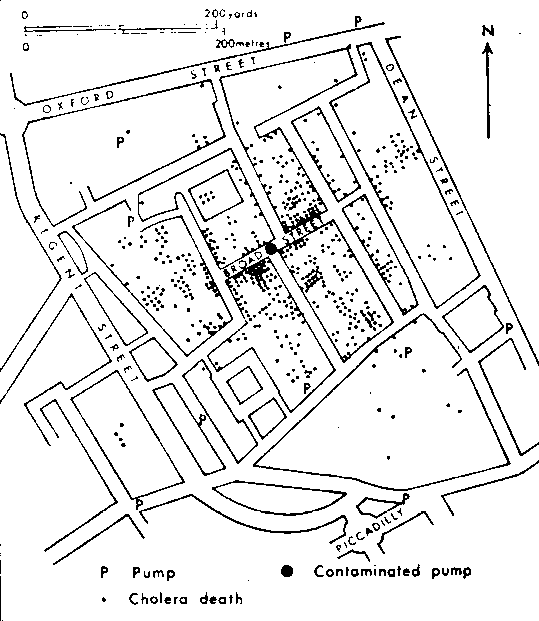
The 1854 outbreak, then, allowed him to further gather data and test his hypothesis--and perhaps obtain his experimentum crucis. Snow, in fact, was ideally suited for this, for a number of reasons. First, his investigations into previous cholera outbreaks taught him how to use demographic data and statistics and relate those to an epidemic. Two, the outbreak just happened to take place in his own neighborhood. This allowed him to do a great deal of first-hand detective work, interviewing cases (or relatives, friends, and neighbors of victims who had died), finding common threads that ran through the stories not only of those who became ill, but also of those that remained well. Though the outbreak was concentrated in his neighborhood, residents in some buildings remained free of disease, while those who lived next door were highly affected. Why? One example was a brewery, where scarcely any cases of cholera had been reported. When Snow asked about the water the employees drank, he found they rarely drank water--they drank malt liquor instead. In another nearby factory, however, a high proportion of workers had become ill or died--and Snow found they gave their employees water from a pump he'd already suspected was at the root of the outbreak. Armed with data about cases of disease and supply of drinking water in the neighborhood, Snow finally felt he had proved his case. Slowly, others would eventually be won over.
While John Snow's story is the central thrust of The Ghost Map, Johnson does just what Christine Gorman suggested journalists should do--he looks at it from all levels, from the microscopic (the causative organism, Vibrio cholerae), to the macroscopic (sanitation, sewage, the very infrastructure of cities). All played a role--and continue to play a role--in cholera outbreaks. Though many in public health will already be familiar with the general story of John Snow (and others who played a role, including Reverend Henry Whitehead, who pinned down the index case that began the outbreak), Johnson does much more than just re-tell Snow's story. He puts it in the much larger context of how we deal with sanitation in general, and how that continues to affect urban planning 150 years after Snow's research. Sadly, he also demonstrates that in parts of the world today, little has changed since John Snow's London.
Further reading
Steven Johnson, The Ghost Map. Riverhead Books: 2006.
All about John Snow, UCLA Department of Epidemiology.
Image from http://www.york.ac.uk/depts/maths/histstat/images/snow_map.gif

Tara writes:
The circulatory system...a system so fascinating he had to study it twice.
JK :)
In an interesting case of synchronicity, History Channel aired a show "Cities of The Underworld", witch discussed this very subject! They showed the "host" walking through tunnels beneath London, and walking along the covered rivers, which back in the cholera plague days were uncovered. Thanks for your much more detailed look at this!
Ms Smith,
your formulation "the circulatory system, and the circulatory system", while logically impeccable, is probably not what you intended to write. Should one of them be some other system?
Jim Roberts
Oops! I see that this has been mentioned already. Sorry!
Ah, yes. But the experimentum crucis was done some years later by Max von Pettenkofer, one of ht great materialists of the 19th century. He (and his students!) drank cholera bacillus obtained from his friend Prof. Gaffky who obtained it from a freshly fallen case during the 1892 Hamburg epidemic. He also took care to drink some antacid first to neutralize his stomach acid. Result of the crucial experiment? All the subjects were fine (as I recall there was one case of light diarrhea). Science isn't always so simple.
I read The Ghost Map and liked it quite a bit, although it has some idiosyncrasies. But I think it overstates Snow's immediate influence. Even in the 1880s his views were only one of many, as Pettenkofer and his competing grundwasser theory shows.
Dr. Smith, your post is a wonderful example of the scientific method. I am a high school science teacher and I can't wait to share your insight of science observation gone wrong, and how it was then done right, with my students. Thank you.
My understanding from the book and other sources wasn't that Miasma made much logical sense at all. The problem was the visceral reaction to the smells of London. Something that smelled that vile had to be bad for you? Right? The sections describing London life; Tanneries, mud-larks, rag and bone men, nightsoilmen and the cesspools was particularly useful for trying to imagine what the place smelled like then.
I took this as a lesson that your emotional or first reaction to a complex problem should be ignored in favour of careful analyses of the empirical data. Just because it 'feels' right doesn't mean that it is right.
Would John Graunt of mid-17th century London get any credit as a proto-epidemiologist, in his Observations on the Bills of Mortality?
Also, if you get a chance to see Anthony Clavroe's play "The Living", about the 1665 plague and John Graunt, do so. It's a great play.
Sorry, that should be "Anthony Clarvoe", not Clavroe.
Cholera epidemics hit New York City three times in the XIXth century, when my family was in the process of moving into the City from rural New Jersey. We were fortunate to have escaped it.
The poor sections of the City were hit the hardest in 1832 and 1849, and the more well-to-do assumed it was the moral depravity of the poor immigrants and African-Americans that brought on the epidemic. Some ministers said it was God's punishment for immorality. (Sound familiar?) The fact that the better off caught the disease, too, was conveniently glossed over or blamed on their proximity to the poor.
Snow's work led the City fathers to clean up, literally, so that the effects of cholera in 1866 were minimized. And of course there were no more epidemics once NYC had decent sanitation and sewage systems.
Details are here at the CUNY site, if you're interested: http://www.virtualny.cuny.edu/cholera/cholera_intro.html
What does that guy Crowe have to say about cholera?
Dang it. :) I forget what I was going to write, so I'll just eliminate the redundancy. Thanks for the catch.
I drink quite frequently in the John Snow pub (primarly because of the cheap beer prices when compared to the rest of London), just over the road from the pump. I believe there is an annual med school pilrimage there.
http://www.johnsnowsociety.org/