It's just not been Vegas' week. First a ricin-laced hotel room, then a clinic-associated outbreak of hepatitis C virus (and potentially hepatitis B and HIV) that could become enormous. Meanwhile, an outbreak of
The group of hepatitis viruses (A, B, C, D, E, and G) are related in name only. They've all been either associated with or found to cause hepatitis--inflammation of the liver. This can be acute inflammation (short-lived; lasting less than ~6 months) or it can become chronic--persisting for years. Chronic infection with these viruses can also lead to liver cancer; in fact, infection with hepatitis B or C is one of the most important risk factors for primary liver cancer.
Hepatitis A
As far a human disease goes, the beginning of the hepatitis virus alphabet soup cause, by far, the most morbidity and mortality. Hepatitis A is a picornavirus with a single-stranded RNA genome. Hepatitis A is unique among the hepatitis viruses when it comes to transmission and disease manifestation. Like the related polio virus, the primary route of transmission is through the fecal-oral route. Outbreaks of the virus have occurred primarily due to food which has been contaminated with fecal material. This virus also differs from B and C in that it's not been shown to cause a chronic manifestation of disease. There is, however, a vaccine available.
Hepatitis B
Hepatitis B virus is a DNA virus, and by far the most prevalent of the hepatitis viruses. It's estimated that a third of the world's population has been exposed, and between 3-6% are infected at any one time. Transmission is known to occur from exposure to blood and body fluids--via sex, injection drug use or other blood exposure, and during pregnancy and breast feeding. Prevalence varies worldwide, with the highest rates in Africa, China, and parts of South America.
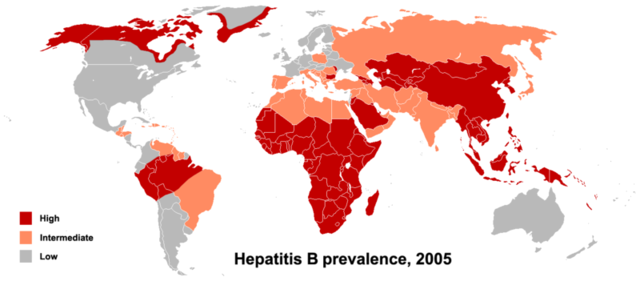
Not coincidentally, these areas also have high rates of liver cancer, as HBV is a main risk factor for the development of this cancer. However, as with the hepatitis A virus, a vaccine is also available. Though the HPV vaccine gets a lot of press as the "first cancer vaccine," HBV truly should have that claim to fame. However, the HBV vaccine has also had its own share of controversy. For one, because--like HPV--hepatitis B can be transmitted sexually, there was some resistance to having infants vaccinated against a sexually-transmitted disease. Second, rates of HBV infection in the United States are fairly low, so some argues that the HBV vaccine was an unnecessary vaccine in this country. However, acquiring an HBV infection in infancy makes it much more likely the infection will become chronic.
Hepatitis C
Previously known as "non-A, non-B" infectious hepatitis, the hepatitis C virus was discovered in the late 1980s (after being hypothesized to exist based on the epidemiology of transplant-associated hepatitis since at least the 1970s). Hepatitis C is a flavivirus with an RNA genome, related to the viruses that cause yellow fever and dengue.
The transmission of hepatitis C is similar to that of HBV: transmitted mostly by blood and sex, although blood-borne transmission (especially injection drug use) seems to be the main route of spread. Worldwide, it's estimated that 150-200 million people are infected with this virus, including 35-185,000 new cases every year in the U.S.--and there's no vaccine for this one. However, treatment is possible, with interferon alpha and ribavirin (the latter may need to be taken for almost an entire year to be effective). Morbidity and mortality are even more severe when an individual is co-infected with more than one of the hepatitis viruses, and hepatitis C infection has also been found to increase the risk of subsequent development of liver cancer.
Hepatitis D
The hepatitis D virus is another RNA virus; however, alone the virus is essentially a non-entity, as it can only replicate when the hepatitis B virus is also present. Though the virus doesn't cause any pathology on its own, when present in conjunction with HBV, their combined presence causes an increased mortality rate (up to 20% of those infected).
Hepatitis E
Hepatitis E is another RNA virus, similar in many ways to Hepatitis A, especially because its main mode of transmission is via the fecal-oral route and from contaminated food and water. Also like Hepatitis A, it doesn't appear to have a chronic stage. Though mortality is typically low, deaths occurring as a result of a large-scale outbreak can be higher than during endemic infection. Additionally, mortality can be very high in women who are in late stages of pregnancy: up to 20% of women who are infected in their third trimester die. Hepatitis E is unique, however, in that it can be zoonotic: in addition to humans, it can infect many species of livestock, as well as non-human primates (and, apparently, rats in the United States).
Human Hepatitis E infection is quite uncommon in the United States; the cases we see here are mainly in travelers who contracted the infection outside of the country. It is more frequently seen in parts of Africa, Asia, and south of our border in Mexico. Currently, an outbreak of Hepatitis E is simmering in Uganda, resulting in over 300 cases and 11 deaths thus far since the outbreak began in November.
Hepatitis G
Finally, another RNA virus, Hepatitis G, rounds out our alphabet soup of hepatitis viruses. However, there's uncertainty about whether the virus causes any clinical symptoms at all, although it was first associated with clinical hepatitis when identified just over a decade ago. Hepatitis G (also known as GB virus C) is related to Hepatitis C, and transmitted via blood and sex like HBV and HCV. However, unlike the synergistic effects one sees when a patient is infected with two type of hepatitis viruses, infection with both Hepatitis G and Hepatitis C appears to slow the progression of liver disease. Similarly, some studies have shown that HIV+ individuals who are co-infected with Hepatitis G likewise show prolonged survival with AIDS than an uninfected comparison group (though it should be noted this remains controversial, and it's unsure whether the virus is directly affecting this or if it's simply a marker for something else).
What the heck happened in Vegas?
So, now that we have some background on the various hepatitis viruses, back to Vegas. It appears that, even in this day and age in a developed country, people are still re-using injection equipment:
The city of Las Vegas shut down the Endoscopy Center of Southern Nevada last Friday after state health officials determined that six patients had contracted hepatitis C because of unsafe practices including clinic staff reusing syringes and vials. Nevada health officials are trying to contact about 40,000 patients who received anesthesia by injection at the clinic between March 2004 and Jan. 11 to urge them to get tested for hepatitis C, hepatitis B and HIV.
The clinic director took out an ad in the local newspaper to discuss the situation and express sympathy for the fear the patients must be experiencing, but denies that supplies were re-used:
"The evidence does not support that syringes or needles were ever reused from patient to patient at the center," Desai wrote.
He leaves unexplained how 5 of the patients, whose infections were traced back to a visit on the clinic on the same day, managed to have phylogenetically-related viruses. That evidence supports the assertion that someone seriously messed up. Whether this may just be the "tip of the iceberg" in that other clinics may be similarly re-using materials remains an open question--and a truly inexplicable one given our knowledge of blood-borne pathogen transmission, and prevention thereof.
Image from http://upload.wikimedia.org/wikipedia/commons/thumb/0/09/HBV_prevalence…
- Log in to post comments

So what happened to hepatitis F, you ask? I couldn't stand the suspense myself, so I looked it up. It seems the hep F exists solely in the realm of hypothesis, with many potentially suspect cases but never a virus isolated.
Hmmm, can something be potentially suspect? That's like a possible maybe.
I was wondering the same thing. Thanks
I work at a needle exchange, and my understanding of Hep C is that the virus can survive for a good amount of time outside of the body, that is to say the clinic director could be right about reuse of points et al., and the transmission still could have happened there. In that way Hep C's not at all like HIV, and prevalence numbers among IDUs tend to show much higher HCV percentages than HIV. Our recommended injection procedures focus on preventing HCV transmission on the assumption that if you stop that, HIV doesn't stand a chance of surviving.
It wouldn't make me feel any better if I were a client of this clinic, but does anyone know if the prep was done in a sterile area with sterile hands, surfaces and instruments? The outbreak could obviously have happened because of point reuse; I'm just saying there may be other vectors as well.
I really doubt anyone cares about these obscure viruses, that remarkably seem to multiply in number (Hep A, Hep, B, Hep C, Hep D, Hep E =>>>>> Hep ZZ)as middling, mediocre scientists strive to find something, anything, to write about in order to get funding.
Mountain Man is silly. When 3% of the world's population is infected with Hep C, that's a big problem. When the percentage of Hep C infection in Egypt is 15%, that's a big problem. In fact, I think the case of Egypt made people aware of the possibility of infectious disease spreading through contaminated needles. That's why every shot you take nowadays is disposable. The case of Egypt is medical and humanitarian tragedy, and yet Mountain Man dismisses it by saying the study of hepatitis viruses is somehow insignificant. Hepatitis viruses cause death and disease-- that alone should make it significant. Moreover, a virus doesn't have to be medically significant to justify study; any scientist would rant similarly, but in a more barbed and long-winded fashion.
I could go on, but Mountain Man is silly, and I don't need to say more to point that out.
The inhabitants of northern North America (Inuits, or the population as a whole?) seem to have a high risk of Hep B. Is it sex? Needles? Eating raw seal meat? What is the risk factor for this population?
Re Dunbar
Mr. Mountain Man, like his fellow clowns cooler and Kevin is a world class denier, vis HIV/AIDS, Global Warming, efficacy of vaccines, etc. He is typical of whackjobs who lurk the net posting the dumbest garbage imaginable. Having nothing better to do as they have no lives, they at least provide amusement with there ravings.
Obscure viruses? Are you kidding?
This must be why antivaccination lunacy is so prevalent. If someone doesn't actually get a disease themselves they think they're rare or unimportant.
And there probably isn't another Hepatitis virus. A non A-E (F) has been proposed to explain sporadic hepatitis but no other infectious agent is known. It is likely these cases are being cause by toxic exposures or some other idiopathic phenomenon.
Finally in terms of needle transmission Hep B is by far the most virulent, but luckily due to widespread vaccination of healthcare workers it is less likely to be a problem these days. I recall something along the lines of a needlestick giving you ~ 1:10 chance of transmission. Hep C is far less likely to transmit by needlestick alone than B (something on the order of 5-10 x less), and HIV is even more fragile outside the body usually requiring blood to be transmitted (as when IV drug users pull blood into a syringe to check patency of a vein). A simple needlestick is dangerous though and healthcare workers have been infected through needlesticks despite the relatively lower risk compared to the hepatitis viruses but the number we're quoted in training is something on the order of a 1:250 risk of HIV transmission if merely stuck by a positive needle.
SLC and hoofnagle, why dont you guys summarize in your own words the original scientific papers that proved hepatitis C is pathenogenic in humans, or is this another no animal model 1/1000 cell 20 year window period virus that was a money making scam by Chiron, when the true cause is just drugs and alcohol.
just post the original scientific experiments from pub med that proved hepatitis C is the cause of progressive liver failure and not drugs and alcohol.
B. Hepatitis C Virus and Non-A Non-B Hepatitis
Non-A non-B hepatitis is observed primarily in recipients of transfusions and in intravenous drug users (3, 12, 160). It has been postulated to be a viral disease because inoculation of plasma or serum (3-75 ml) from hepatitis patients into chimpanzees induced some biochemical markers of hepatitis, such as alanine aminotransferase, in half of the animals (160). However, none of the animals developed hepatitis (161, 162). Trace amounts of presumably viral RNA have recently been detected in the liver of hepatitis patients. In addition, "nonneutralizing" antibodies to "nonstructural epitopes," from an apparently latent RNA virus, have been identified mostly in asymptomatic carriers (160). Cloning and sequencing indicated that the RNA is directly coding and measures about 10 kb. Therefore, the suspected virus has been tentatively classified as a togavirus (160). Viral RNA was only detectable after amplification with the PCR in 9 out of 15 non-A non-B hepatitis patients, and non-neutralizing antibodies were found in only 7 of the 9 RNA-positive and in 3 of the 6 RNA-negative patients (163). Likewise, liver tissues from chimpanzees inoculated with sera from hepatitis patients contain only one viral RNA molecule per ten cells (160).
In view of this evidence, the putative virus has been termed hepatitis C virus (HCV) to indicate that it is the cause of the hepatitis. Subsequently, the Food and Drug Administration has recommended, and the American Association of Blood Banks has mandated, as of 1990, the testing of the approximately 12 million annual blood donations in the U.S. (82) for antibodies to HCV at an approximate cost of $5 per test. The test was developed by Chiron Co., Emeryville, California (Irwin Memorial Blood Bank, personal communication, August 15, 1991).
However, several arguments cast doubt on the hypothesis that HCV causes hepatitis:
1. Virus-containing sera or plasma from hepatitis patients does not cause hepatitis if inoculated into chimpanzees, indicating that HCV is not sufficient to cause the disease. Moreover, since the virus has not been propagated in culture and isolated in a pure form, the possibility exists that the biochemical markers of hepatitis that are observed in chimpanzees inoculated with plasma were induced by another agent. Thus, HCV is not likely to be a sufficient cause of hepatitis in humans.
2. The presence of HCV in asymptomatic subjects at the same concentration and activity as in hepatitis patients also indicates that the virus is not sufficient to cause hepatitis.
3. The absence of viral RNA in 6 out of 15 hepatitis C patients indicates that the virus is not necessary for the disease.
It appears that HCV either causes disease by unprecedented mechanisms with as little as one RNA molecule per 10 liver cells in some and even less in other carriers, or that the virus is not the cause of non-A non-B hepatitis. By contrast, the concentration of viral RNAs made by conventional pathogenic viruses, including togaviruses, ranges from 103 to over 104 per cell (10). Therefore, it seems plausible that a latent passenger virus was identified that survives by establishing chronic asymptomatic infections at very low, nonpathogenic titers (164).
Jesus this Duesberg Character es mi hero!
Cooler, your source is a review article from 1992. Specifically, Duesberg PH and Schwartz JR Latent viruses and mutated oncogenes: no evidence for pathogenicity. Progress in Nucleic Acid Research and Molecular Biology 43:135-204, 1992.
There have been nearly 37,000 articles published about hepatitis C since the end of 1992. The virus has been extensively studied in chimps (the same virus) and it definitely causes both chronic hepatitis and hepatocellular carcinoma.
About a decade ago around the south San Francisco bay, they fired a clinic worker for reusing needles. There have been other instances elsewhere in the country.
If you don't see the needle removed from an unopened package, ask for another.
Seems like if I was right another no animal model 1/1000 cell 20 year window period virus. Seems like Drugs and alcohol are a more likely cause than hepatitis C. But a drug company said it causes it, Chiron, so it must be true!
"Using chimpanzees has presented numerous problems in that they appear to respond to HCV differently than humans. Mother-infant transmission has been reported in humans but not chimpanzees.(1) Chronic infection occurs approximately 75% of the time in humans but only 30-50% of the time in chimpanzees.(2,3) Humans progress to liver fibrosis and cirrhosis while chimpanzees do not. This may in part be due to environmental differences between the species; e.g., humans consume large quantities of alcohol while chimpanzees do not. Other environmental differences also exist. Humans suffer from hepatocellular carcinoma as a result of HCV. Hepatocellular carcinoma after HCV infection is very rare in chimpanzees.(4) The course of HCV is highly variable in the chimpanzee, as it is in humans, but is the variability secondary to the same causes in both species?"
Hep C is another of these bullsheet diseases that the scientists and pharmaecuetical and international health bureucrats keep inventing.
Look, to sell products and make money, McDonnell-Douglas, Hughes Aircraft, Halliburton and Boeing need war.
To sell products and make money, Merck, Pfizer, Gilead, Schering-Plough need disease. It's just that simple.
Avian bird flu, SARS, AIDS, Hep C, West Nile, Ebola -- it's all crap. Heart disease, cancer, stroke, accidents -- those are the real diseases in America.
In poor countries like Africa, basically they need better sanitation, cleaner water and nutrition, not a buncha toxic junk to combat phantom microbes.
The more I think about it, the more I understand how utterly incompetent, disgraceful and greedy the microbe-hunters really are. They are modern-day alchemists reading the entrails of microscopic bugs.
Totally agree Mountain man. And when an a good scientist truly does prove a microbe is pathenogenic in humans he gets ignored because he's not supported by a drug company or a crooked politician, this microbe has already spread to the general population, and they are left to rot and die.
And then you people wonder why I worship Dr. Shyh ching lo, a big supporter of Duesberg in the early 90's, we shall have a moment of silence for Dr. Lo, this is how you prove a microbe causes disease in humans.......
Histopathology and doxycycline treatment in a previously healthy non-AIDS patient systemically infected by Mycoplasma fermentans (incognitus strain).Lo SC, Buchholz CL, Wear DJ, Hohm RC, Marty AM.
Department of Infectious and Parasitic Diseases Pathology, Armed Forces Institute of Pathology, Washington, D.C. 20306-6000.
The newly recognized human pathogenic mycoplasma M. fermentans (incognitus strain) causes a fatal systemic infection in experimental monkeys, infects patients with AIDS, and apparently is associated with a fatal disease in previously healthy non-AIDS patients. An apparently immunocompetent male who lacked evidence of HIV infection developed fever, malaise, progressive weight loss, and diarrhea and had extensive tissue necrosis involving liver and spleen. M. fermentans (incognitus strain) was centered at the advancing margins of these necrotizing lesions. Following the treatment of 300 mg doxycycline per day for 6 weeks, he recovered fully. He has no fever or diarrhea, and his abnormal liver function tests have returned to normal. He regained all lost strength and 14 kg of lost weight and has remained disease free for more than 1 year.
PMID: 1788266 [PubMed - indexed for MEDLINE]
Hey Cooler,
By the way, HCV has been classified as a Flavivirus. It helps if you stay current (you know, in the present century) with your cutting and pasting.
Ever think that maybe the Hep C virus and other viruses has mutated/evolve to favor infection in humans - you know humans engage in more behaviors likely to favor infection and viral replication? Ever heard of species specificity?
Hey, by the way, HCV can know be grown in cell culture. Just another reason to stay current with your cutting and pasting.
ooooooooooooooooooooh a flavivirus oooooooooooohhhhhhhhhhhhhhhhhhhhhhhhhhhhh im so scared. ooooooooooooooooooooooooooooooooh. Honestly im much more scared of getting 100 times the epa safe amount of mercury in a flu shot or getting some Project day lily weaponized mycoplasma in my life.
So how long has the window period been extended for Hep c is it ten years, or are we up to 40 years as in the case with HPV? Oh I'm sorry, there are ads for HPV on TV by Merck so it must be true!
If you are so sure Hep C is the cause of progressive liver failure, provide the orginal scientific papers that proved this, they should be from the early 90's for that was when every doctor was taught in medical school it was the cause and the blood supply was screened etc. Waiting for those papers, you guys might have to think for yourselves on this one, because theres no NIH factsheet on this one!
Cooler, please cite your sources. I found that piece only at a site dedicated to eliminating the use of animal models (http://www.curedisease.com/articleHCV.html) and it seems to be mostly intended to encourage cell culture systems. (There are multiple in vitro models, at this point, but you don't believe in those.)
Koch's postulates are fulfilled by Hep C virus (Lindenbach et al. 2006, PNAS 103(10):3805-9). You need to let this one go, because you're wrong.
Hey thanks Jen m for that study! Did you bother reading the results? You need to let this one go Jen, because you're wrong.
Results
"HCVcc Is Infectious in Chimpanzees. We investigated whether HCVcc strain FL-J6/JFH would be infectious in vivo by inoculating two HCV-negative chimpanzees via i.v. injection with 1 x 106 tissue culture infectious doses (50% endpoint, TCID50). Both animals exhibited a rapid rise in viremia, peaking between 104 and 105 international units (IU) of HCV RNA per ml of plasma within 2 weeks postinfection (Fig. 1A). After an acute viremic phase, the viral load in chimpanzee 4x0483 decreased but was maintained between 102 and 104 IU/ml for 17 weeks before dropping below the limit of detection. In contrast, the viral load in chimpanzee 4x0495 became undetectable by week 7 then reappeared briefly at week 15. Neither animal exhibited clinical signs of hepatitis or elevated serum alanine aminotransferase (ALT) and aspartate aminotransferase (AST) throughout 4 months of observation (Fig. 1A). These data demonstrate that HCVcc is capable of establishing infection in vivo and that the virus can persist in these animals for at least several weeks."
None of the chimpanzees developed any sign of liver deteroration, even after they were frankensteined in the labratory to have "human liver grafts." Did Koch say you could frankenstein animals to prove pathenogenicity? Well even if he did, it failed in this case!
"Neither animal exhibited clinical signs of hepatitis or elevated serum alanine aminotransferase (ALT) and aspartate aminotransferase (AST) throughout 4 months of observation"
Lindenbach BD, Meuleman P, Ploss A, Vanwolleghem T, Syder AJ, McKeating JA, Lanford RE, Feinstone SM, Major ME, Leroux-Roels G, Rice CM.
Center for the Study of Hepatitis C, Laboratory of Virology and Infectious Disease, The Rockefeller University, 1230 York Avenue, New York, NY 10021, USA.
Hepatitis C virus (HCV) is a major cause of chronic liver disease, frequently progressing to cirrhosis and increased risk of hepatocellular carcinoma. Current therapies are inadequate and progress in the field has been hampered by the lack of efficient HCV culture systems. By using a recently described HCV genotype 2a infectious clone that replicates and produces infectious virus in cell culture (HCVcc), we report here that HCVcc strain FL-J6/JFH can establish long-term infections in chimpanzees and in mice containing human liver grafts. Importantly, virus recovered from these animals was highly infectious in cell culture, demonstrating efficient ex vivo culture of HCV. The improved infectivity of animal-derived HCV correlated with virions of a lower average buoyant density than HCVcc, suggesting that physical association with low-density factors influences viral infectivity. These results greatly extend the utility of the HCVcc genetic system to allow the complete in vitro and in vivo dissection of the HCV life cycle.
PMID: 16484368 [PubMed - indexed for MEDLINE]
Even when they tried to frankenstein mice with human liver grafts they failed. Jen m you gonna admit you guys have no idea what you're doing? I suggest you scroll up and learn from Dr. Lo how to prove pathenogenicity in humans.
"In situ PCR and immunohistochemistry clearly demonstrated positive signals for HCV in the cytoplasm of infected hepatocytes, while the engrafted human liver tissues showed no apparent morphological changes indicative of infection"
Hepatitis C virus infection in human liver tissue engrafted in mice with an infectious molecular clone
Norio Maeda11Department of Internal Medicine, School of Medicine, Keio University, Tokyo, Japan, , Mamoru Watanabe22Department of Gastroenterology and Hepatology, Graduate School, Tokyo Medical and Dental University, Tokyo, Japan, , Susumu Okamoto11Department of Internal Medicine, School of Medicine, Keio University, Tokyo, Japan, , Takanori Kanai22Department of Gastroenterology and Hepatology, Graduate School, Tokyo Medical and Dental University, Tokyo, Japan, , Taketo Yamada33Department of Pathology, School of Medicine, Keio University, Tokyo, Japan, , Jun-ichi Hata33Department of Pathology, School of Medicine, Keio University, Tokyo, Japan, , Nobumichi Hozumi44Research Institute for Biological Sciences, Science University of Tokyo, Tokyo, Japan, , Asao Katsume55Department of Microbiology and Cell Biology, Tokyo Metropolitan Institute of Medical Science, Tokyo, Japan, , Hideko Nuriya55Department of Microbiology and Cell Biology, Tokyo Metropolitan Institute of Medical Science, Tokyo, Japan, , Jasbir Sandhu66Department of Surgery, Faculty of Medicine, University of Toronto, Toronto, Canada, Hiromasa Ishii11Department of Internal Medicine, School of Medicine, Keio University, Tokyo, Japan, , Michinori Kohara55Department of Microbiology and Cell Biology, Tokyo Metropolitan Institute of Medical Science, Tokyo, Japan, and Toshifumi Hibi11Department of Internal Medicine, School of Medicine, Keio University, Tokyo, Japan, 1Department of Internal Medicine, School of Medicine, Keio University, Tokyo, Japan, 2Department of Gastroenterology and Hepatology, Graduate School, Tokyo Medical and Dental University, Tokyo, Japan, 3Department of Pathology, School of Medicine, Keio University, Tokyo, Japan, 4Research Institute for Biological Sciences, Science University of Tokyo, Tokyo, Japan, 5Department of Microbiology and Cell Biology, Tokyo Metropolitan Institute of Medical Science, Tokyo, Japan, 6Department of Surgery, Faculty of Medicine, University of Toronto, Toronto, Canada
Toshifumi Hibi, Department of Internal Medicine, Keio University School of Medicine, 35 Shinanomachi, Shinjuku-ku, Tokyo 160-8582, Japan.
Tel: 81-3-3357-6286
Fax: 81-3-3357-6156
e-mail: thibi@sc.itc.keio.ac.jp
Maeda N, Watanabe M, Okamoto S, Kanai T, Yamada T, Hata J, Hozumi N, Katsume A, Nuriya H, Sandhu J, Ishii H, Kohara M, Hibi T. Hepatitis C virus infection in human liver tissue engrafted in mice with an infectious molecular clone.
Liver International 2004: 24: -. © Blackwell Munksgaard 2004
Abstract
Abstract: Background/aims: Recent advances in molecular cloning of hepatitis C virus (HCV) have enabled us to apply some available HCV molecular clones to experimental studies. However, these investigations have been restricted to chimpanzee models or 'isolated hepatocytes' from tree shrews. In this study, we engrafted 'human liver tissue' into immunodeficient mice and investigated HCV infection using an infectious molecular clone.
Methods: Human liver tissues from normal (non-HCV-infected) liver were transplanted into non-obese diabetic/severe combined immunodeficiency (NOD/SCID) mice. We then inoculated the mice with sera from HCV-infected patients or an infectious HCV molecular clone. HCV RNA was assessed using nested reverse-transcription polymerase chain reaction (PCR), real-time detection PCR and in situ PCR.
Results: Without any growth support, normal human liver tissues survived in NOD/SCID mice while maintaining the original viable hepatic architecture. HCV RNA was detected in the mice serum until the fourth week after the inoculation. In situ PCR and immunohistochemistry clearly demonstrated positive signals for HCV in the cytoplasm of infected hepatocytes, while the engrafted human liver tissues showed no apparent morphological changes indicative of infection.
Conclusion: Engraftment of human liver tissues into NOD/SCID mice and infection with HCV molecular clones could offer a reverse genetic strategy for HCV infection.
Sorry, the chimpanzees didnt not recieve "trnasplanted human liver grafts", only the mice, either way neither of them developed hepatitis, when inoculated with hep c, no sign of liver damage, inflammation, or even elevated liver enzymes at all! What a joke!
When you guys let drug comapanies like Chiron control your minds, this is what happens, millions of people are told they are going to die with Hepatitis C when there is no evidence for it, and the real cause is probably just poor habits like alcoholism and drug abuse etc.
Cooler has been rolling all over the floor laughing at these quotes that reveal the hepatitis c fraud!
"Neither animal exhibited clinical signs of hepatitis or elevated serum alanine aminotransferase (ALT) and aspartate aminotransferase (AST) throughout 4 months of observation"
"In situ PCR and immunohistochemistry clearly demonstrated positive signals for HCV in the cytoplasm of infected hepatocytes, while the engrafted human liver tissues showed no apparent morphological changes indicative of infection."
Nobody's saying Kochs postulates are perfect, but when a drug companies microbe fails all of them and has all the charecteristics of a harmless passenger virus (most microbes are harmless), and none of a pathenogenic one makes for one good laugh!
While on the topic of hepatitis;
Hows about some drug-induced hepatitis and death with that Prezista?
To the Tara et al gang... how can you be such staunch supporters of such fucking lunacy?
Jen's reference was to the successful culturing of HCV in vitro, followed by successful inoculation. This is what Cooler, unwisely believing the dilettantish Duesberg, thought had not been done.
Cooler is correct, though, in observing that the inoculated animals did not develop liver disease. Chimps exposed to some strains of HCV do exhibit higher liver enzyme levels, but they did not in this particular study of this particular virus.
In fact, chimpanzees typically do not show the same symptoms as some infected humans....at least partly due to the fact that HCV's effects often exert themselves over decades in humans, and forty-year experiments in large groups of chimpanzees are difficult in any funding environment.
Can a virus (or bacterium, or fungus) be said to cause disease only if it is present in every case of disease? Only if every infection leads invariably to disease? Only if every animal species inoculated becomes infected and proceeds to disease?
If so, no replicating agent causes disease; not even Cooler's beloved Mycoplasma, which was found by Montagnier (and others) in plenty of healthy controls. Nor does any drug cause disease, since many drug users do not have AIDS, cirrhosis, etc. Nor do carcinogens cause cancer (remember the two-pack-a-dayer who died in his sleep at 103), or high-fat and cholesterol diets lead to heart disease. Nor can any vaccine be implicated in adverse events, since most recipients have none.
With the bar raised this high, no cause has effect in the biological realm.
Thanks to Carter for the Prezista link. Out of curiosity:
How many deaths have occurred in patients on Prezista?
How many deaths in matched patients (same symptoms, same non-Prezista drugs) not on Prezista?
How many of the Prezista deaths or hepatitis cases were in patients with advanced AIDS? With Hep B and/or C? With cirrhosis?
Is there evidence Prezista hastened the deaths of any patients?
Is there an animal model of Prezista-induced liver damage and death?
To Carter and Cooler, a handful of chimpanzees that "only" have elevated liver enzyme levels on infection with HCV means HCV is a hoax and does not cause disease in people, but if several very sick people who take a particular drug die, that drug must be a lethal poison.
Lo between his patents and publications did not find mycoplamsa incognitus/penetrans in over a hundered healthy controls. Montagnier found high titer of antibodies to m penetrans in aids patients who usually had a lower t cell count.
http://cvi.asm.org/cgi/reprint/4/6/787.pdf
Elk mountain..
you know this is just one typical thing after another with the mainstream. The drugs dont work the vaccines are an utter failure, and they screem for more money. It's just time to give up HIV - dont ya think?
Hepatitis C, another illness where people are told they are going to die with no evidence at all, they can never engage in a relationship, friends will abandon them, all because Chiron pushed it on the public, and the disgraceful CDC and thier mindless sycophants ruined millions of more people's lives.
If you scroll up you will see you guys have provided no evidence that hepatitis c causes progressive liver failure, and when that evidence was provided, it was fallacious and inaccurate, like when Jen m provided a study she claimed folfilled Koch's postulates for Hep c, the results showed that no chimpanzee deveopled any sign of liver illness! I hope this was an accident, and not a deliberate attempt that I would not read the entire study.
It's amazing the way you guys operate, keeping secrets, not giving patients any informed consent, if most people had a cursory undertanding of Koch's postulates and the crooked ways these microbes were brought to the public realm by unscrupulous drug companies and 2nd rate scientists, theyd dump the HPV, HEP C dogma overnight.
Even when they gave IMMNUNODEFICIENT mice human liver grafts and then inoculated them with hep C nothing happened in that Japanese study! Even after they extended the goalposts as much as they could they failed!
"In situ PCR and immunohistochemistry clearly demonstrated positive signals for HCV in the cytoplasm of infected hepatocytes, while the engrafted human liver tissues showed no apparent morphological changes indicative of infection."
Hepatitis C virus infection in human liver tissue engrafted in mice with an infectious molecular clone
Norio Maeda11Department of Internal Medicine, School of Medicine, Keio University, Tokyo, Japan.
How do you guys sleep at night perpetuating this fraud?
cooler, as I've mentioned previously, it's you who lack understanding of Koch's postulates. Heck, read the wiki entry which specifically mentions Hep C, as well as how Koch himself modified his own postulates when he discovered (gasp!) exceptions. Microbiology did not screech to a halt in 1900, and there are other criteria for determination of causation--look up Bradford-Hill criteria, for instance.
Great, I was just going to start playing with my Shyh Ching Lo bobblehead doll, but now I have to respond to this.
I never said Koch's postulates were perfect, I just want you to provide me with the scientific papers that overwhelmingly prove Hep C causes liver disease and not drugs, alcohol and Factor v111.
How long have you guys extended the symptomless window period for HEP C now, I think we are at about 20-30 years now. Waiting for those papers that prove Hepatitis C is the cause of liver failure and not drugs, alcohol etc. If you don't provide me with those papers, your conceding what the modern day prophet Duesberg said about Hep c years ago in his book "Inventing the Aids Virus".........that the whole thing was a scam by A drug company.
"A third type of hepatitis was found in the 1970s, again restricted to heroin addicts, alcoholics, and patients who have received blood transfusions. Most scientists assumed these cases were either hepatitis A or B, until widespread testing revealed neither virus in the victims. Roughly thirty-five thousand Americans die each year of any type of the disease, a fraction of those from this "non-A, non-B hepatitis," as it was known for years. Today it is called hepatitis C. This form of hepatitis does not behave as an infectious disease, for it rigidly confines itself to people in well- defined risk groups rather than spreading to larger populations or even to the doctors treating hepatitis patients. Yet virologists have been eyeing the disease from the beginning, hoping one day to find a virus causing it.
That day arrived in 1987. The laboratory for the job was no less than the research facility of the Chiron Corporation, a biotechnology company located directly across the bay from San Francisco. Equipped with the most advanced techniques, a research team started its search in 1982 by injecting blood from patients into chimpanzees. None of monkeys contracted hepatitis, although subtle signs vaguely resembling infection or reddening did appear. For the next step, the scientists probed liver tissue for a virus. None could be found. Growing desperate, the team fished even for the smallest print of a virus, finally coming across and greatly amplifying a small piece of genetic information, encoded in a molecule known as ribonucleic acid (RNA), that did not seem to belong in the host's genetic code. This fragment of presumably foreign RNA, the researchers assumed, must be the genetic information of some undetected virus. Whatever it was, liver tissue contains it only in barely detectable amounts. Only about half of all hepatitis C patients contain the rare foreign RNA. And in those who contain it, there is only one RNA molecule for every ten liver cells - hardly a plausible cause for disease.
The Chiron team used newly available technology to reconstruct pieces of the mystery virus. Now they could test patients for antibodies against this hypothetical virus and soon discovered that only a slight majority of hepatitis C patients had any evidence of these antibodies in their blood. Koch's first postulate, of course, demands that a truly harmful virus be found in huge quantities in every single patient. His second postulate requires that the virus particles be isolated and grown, although this supposed hepatitis virus has never been found intact. And the third postulate insists that newly infected animals, such as chimpanzees, should get the disease when injected with the virus. This hypothetical microbe fails all three tests. But Koch's standards were the furthest thing from the minds of the Chiron scientists when they announced in 1987 that they had finally found the "hepatitis C" virus.
Now more paradoxes are confronting the viral hypothesis. Huge numbers of people testing positive for the hypothetical hepatitis C virus never develop any symptoms of the disease, even though the "virus" is no less active in their bodies than in hepatitis patients. And according to a recent large-scale study of people watched for eighteen years, those with signs of "infection" live just as long as those without. Despite these facts, scientists defend their still-elusive virus by giving it an undefined latent period extending into decades.
Paradoxes like these no longer faze the virus-hunting research establishment. Indeed, rewards are generally showered upon any new virus hypothesis, no matter how bizarre. Chiron did not spend five years creating its own virus for nothing. Having patented the test for the virus, the company put it into production and began a publicity campaign to win powerful allies. The first step was a paper published in Science, the world's most popular science magazine, edited by Dan Koshland, Jr., professor of molecular and cell biology at the University of California at Berkeley. Edward Penhoet, chief executive officer for Chiron, also holds a position as professor of molecular and cell biology at the University of California at Berkeley. The NIH-supported virology establishment soon lent the full weight of its credibility to the hepatitis C virus camp. As Chiron's CEO boasted, "We have a blockbuster product." A regulatory order from the Food and Drug Admin-istration (FDA) to test the blood supply would reap enormous sales for Chiron.
Their big chance presented itself in late 1988 as a special request from Japanese Emperor Hirohito's doctors. The monarch was dying and constantly needed blood transfusions; could Chiron provide a test to make sure he received no blood tainted with hepatitis C? The biotech company jumped at the opportunity, making for itself such a name in Japan that the Tokyo government gave the product its approval within one year. The emperor died in the meantime, but excitement over Chiron's test was fueled when the Japanese government placed hepatitis C high on its medical priority list. Chiron's test kit now earns some $60 million annually in that country alone. By the middle of 1990, the United States followed suit. The FDA not only approved the test, but even recommended the universal testing of donated blood. The American Association of Blood Banks followed suit by mandating the $5 test for all 12 million blood donations made each year in this country - raking in another $60 million annually for Chiron while raising the nation's medical costs that much more. And all this testing is being done for a virus that has never been isolated.
Profits from the test kit have generated another all-too-common part of virus hunting. With Chiron's new income from the hepatitis C test, Penhoet's company bought out Cetus, another biotech company, founded by Donald Glaser, who, like Penhoet, also holds a position as professor of molecular and cell biology at the University of California at Berkeley. And Chiron made an unrestricted donation of about 12 million to the Department of Molecular and Cell Biology at the University of California at Berkeley that generates $100,000 in interest each year.
Unfortunately for Peter Duesberg, who belongs to the same department, his supervisor is yet another professor who consults for Chiron Corporation - and displays little sympathy for Duesberg for challenging modern virus hunting by restricting his academic duties to undergraduate student teaching and by not appointing him to decision-making committees. Such conflicts of interest have become standard fixtures in university biology departments.
The modern biomedical research establishment differs radically from any previous scientific program in history. Driven by vast infusions of federal and commercial money, it has grown into an enormous and powerful bureaucracy that greatly amplifies its successes and mistakes all the while stifling dissent. Such a process can no longer be called science, which by definition depends on self-correction by internal challenge and debate.
Despite their popularity among scientists and their companies, "latent," "slow," and "defective" viruses have achieved only little prominence as hypothetical causes of degenerative diseases before the AIDS era. Their hypothetical role in degenerative diseases, which result from the loss of large numbers of cells, remained confined to rare, exclusive illnesses like kuru and hepatitis C.
However, because latent, slow, and defective viruses cannot kill cells, such "viruses" eventually achieved prominence as hypothetical causes of cancer and thus entered the courts of health care and medical research. The next chapter describes the terms under which these viruses were promoted as causes of cancer and how some of these terms were eventually used to promote latent, slow, and defective viruses as causes of degenerative diseases including, above all, AIDS."
Hi hi hi... Exactly like today's virology nerds creepily and incessantly modifying their hypotheses and definitions to keep their houses of cards - like HIV=Aids for instance - standing up, Koch, as well as that Louis Pasteur imposteur of course, had to modify his postulates because he exclusively found exceptions to the rule.
Wake up, people. Koch postulates have never worked and will never work.
Of course I don't write this for the eyes of you who are reading this in the year 2008. It's only meant for your eyes, yes, you there, who reading these lines in the year 3025. You, who are absolutely convinced all people were so infinitely stupid back in 2008. Not all of them, my friend, not all of them. Some knew. Centuries ago already.
Wow it's been days and nobody can give any evidence that hepatitis C causes liver failure in humans, and not drugs, alcohol and clotting factors. Here is a interesting study for you mindless idiotic drug company shills, Factor v111 causes liver damage when injected into chimps..............but Chiron couldnt pursue this hypothesis because it wouldnt make them any money! So when they examined hemophilliacs with liver problems they ignored the most obvious causes in search of their money making phantom virus. Some of you people are so stupid you'll destroy humanity.
Non-A/non-B hepatitis in experimentally infected chimpanzees: cross-challenge and electron microscopic studies.Bradley DW, Maynard JE, Cook EH, Ebert JW, Gravelle CR, Tsiquaye KN, Kessler H, Zuckerman AJ, Miller MF, Ling C, Overby LR.
Inoculation of eight chimpanzees with factor VIII, factor IX, or "H" strain plasma resulted in enzymatic and histopathologic evidence of non-A/non-B hepatitis in all eight animals. Challenge of two chimpanzees convalescent from factor VIII-induced disease with either factor IX or "H" strain plasma resulted in non-A/non-B hepatitis only in the animal inoculated with factor IX materials. Reciprocal cross-challenge of a chimpanzee convalescent from factor IX-induced disease with factor VIII also produced unequivocal enzymatic and histopathologic evidence of non-A/non-B hepatitis. Cross-challenge of a chimpanzee convalescent from "H" strain-induced non-A/non-B hepatitis with factor VII did not cause a second bout of non-A/non-B hepatitis. These findings suggest the factor VIII materials and "H" strain plasma used in these studies share a common etiologic agent (or agents), but that factor VIII and factor IX may contain two distinct agents. Electron microscopic (EM) examination of thin-sectioned, acute-phase liver biopsies from all but one of the chimpanzees receiving the primary inocula revealed the presence of abnormal hepatocyte cytoplasmic structures previously shown to be associated with non-A/non-B hepatitis. Crystalline structure containing 25 to 30 nm particles were visualized by EM in the cytoplasm of endothelial or Kupffer cells in acute-phase liver biopsies obtained from three chimpanzees inoculated with either factor VIII materials or "H" strain plasma.
Fortunately for cooler, he didn't pay attention to the 1980 Bradley et al study abstract as he pasted it. Typical of papers misunderstood by denialists, the Bradley et al study, almost thirty years ago, provided evidence against virus denialism. Namely, that HCV can cause hepatitis, whether its source is plasma or contaminated blood factors.
All animals receiving 'H' strain HCV (known as NANB Hep in 1980) had enzymatic and histopathologic evidence of non-A/non-B hepatitis. "All but one" animal receiving these inocula had classic signs of acute hepatitis by EM. Animals exposed to contaminated blood products like Factor XIII also developed hepatitis.
The Bradley et al study was published well before one of the "common etiologic agents" of non-A, non-B hepatitis that contaminated some blood factor preparations was identified as HCV.....before blood extracts like Factor VIII were treated to prevent transmission of viruses like HCV or HIV....before recombinant and thus HCV-uncontaminated Factor VIII became widely available for treatments.
Cooler has shown that most Aetiology readers are wise to ignore him: left to his own devices, cooler will (unwittingly) refute himself.
No, the lindenbach study clearly proves that it is not Hepatitis C causing disease in chimpanzees, so it must have been something else, some bad reaction hemophialiacs are having to these agents, this study further confirmed this. Recieving foreign proteins is probably what caused tehse chimps to get liver problems.
"In situ PCR and immunohistochemistry clearly demonstrated positive signals for HCV in the cytoplasm of infected hepatocytes, while the engrafted human liver tissues showed no apparent morphological changes indicative of infection."
Hepatitis C virus infection in human liver tissue engrafted in mice with an infectious molecular clone
Norio Maeda11Department of Internal Medicine, School of Medicine, Keio University, Tokyo, Japan.
Very strange stuff this factor VIII must be.... When it is contaminated with hepatitis C virus it can cause biochemical and histological hepatitis. When it is heat treated to eradicate contaminating viruses, it does not cause biochemical or histological hepatitis.
Yet the only conclusion cooler can reach from all this data is that it is Factor VIII (and not Hepatitis C virus) that causes hepatitis.
It must be so wonderful to live in cooler's world, where evidence and logic can never interfere with blissful ignorance.
Idiot,
did you read the studies above from Lindenbach and Keio University, when they isolated hepatitis C and inoculated it into mice with human liver grafts and chimpanzees there was no sign of liver disease. So it must be some other substance/contaminent that caused the Chimpanzees to develop liver disease in that study, I dont know what it is, but by the process of elimination you can rule out hepatatis C becauase thats been isolated and cloned and the animals didn't develop any sign of liver disease.
cooler,
Were you to show a genuine interest in understanding why you have misinterpreted what you have read in the mouse and chimp studies you cite, I'm sure someone would be happy to explain it to you. But if you want to figure it out for yourself, I'll give you two hints. Mice and chimpanzees live in laboratories under conditions that don't come close to approximating the environment human patients inhabit. Hint 2 is that for many infectious diseases, a large part of the tissue damage is caused not by the infectious agent itself but by the immune system trying to respond to the infectious agent. In that regard, immunodeficiency in a laboratory setting isn't always all bad.
Please ignore the trolls. Thanks for posting this summary, Tara. It can get confusing with all those similar names.
Dale,
Stop making speculations and excuses for microbes that have 40 year window periods, are in one a hundered cells, dont cause the same disease in animals just provide me with an epidemilogical study that people who are infected with hepatitis c and dont have any risk factors like alcohol and drugs etc even get sick, instead of extending the window period into the nex millenium every time your microbes fail.
cooler,
In simple words. people who are infected with HCV are more likely to develop chronic hepatitis than people who aren't, regardless of other environmental factors. I'm not making excuses, I'm telling you what experimental data shows (as opposed to the way that Duesberg thinks things "should happen").
Can you provide me a reference for this long term study that rules out confounders such as drugs and alcohol?
It should read something like this, "Because animals inoculated with hepatitis c dont progress to liver failure and Cancer and the window period for this microbe has been extended to decades we are going to follow Hep c positive people with no other risk factors such as alcohol and drugs to see if Hepatitis C is pathenogenic in humans"
I'm waiting, along with cooler, for a response.
*Crickets*
cooler's once again beating up strawmen. There are ways to control for confounders such as drugs and alcohol use in people who are HepC+--and we do know that these all act synergystically anyway (in other words, that those who are HepC+ and are drinkers often have worse disease and progress quicker than those who only have HepC virus as a risk factor). See, for example, a paper I gave to my class earlier in the year: "Prospective Study of Hepatitis B and C Viral Infections, Cigarette Smoking, Alcohol Consumption, and Other Factors Associated with Hepatocellular Carcinoma Risk in Japan" AJE Vol.151, No. 2 p.131-139.
Sorry to interrupt the denialist flamewars and such but I just wanted to thank Tara for putting up such a great, informative review. I somehow missed it when originally posted. This is a concise yet scholarly treatment of the subject - I had not even known of hep D, E, and G (but not the hippopotamus, I mean, F). Also, very nice relevance to a recent event that was not represented entirely accurately in the MSM. Thanks, professor!
I am wondering the same thing. Thanks