tags: Ask a Science Blogger, male birth control pill, contraceptive
The newest "Ask a Science Blogger" question is; Why is there no birth control pill for men?
 I know that many women say that male birth control pills do not exist solely due to sexual politics, namely, why would a pharmaceutical company devote precious research funding to developing a male birth control pill when they can make so much more money from developing drugs such as Viagra? Because I am limited to 500 words or so, I am not here to argue the sexual politics of this issue, but instead, I am interested to discuss the practical health aspects associated with developing a male birth control pill.
I know that many women say that male birth control pills do not exist solely due to sexual politics, namely, why would a pharmaceutical company devote precious research funding to developing a male birth control pill when they can make so much more money from developing drugs such as Viagra? Because I am limited to 500 words or so, I am not here to argue the sexual politics of this issue, but instead, I am interested to discuss the practical health aspects associated with developing a male birth control pill.
The most obvious fact is that preventing pregnancy in a woman is easy when compared to preventing a man from causing pregnancy. A woman does, afterall, only produce one fertile ovum, or egg, each month, whereas a man expells somewhere in the neighborhood of 120 million sperm with each ejaculation. And we all know that many men ejaculate oh .. once or twice per day, on average.
So, based on this simple biological fact, there are several strategies for preventing unwanted pregnancies from occurring in women; preventing egg and sperm from meeting, preventing the fertilized egg from implanting in the uterus, or preventing the implanted embryo from developing into a full-term pregnancy -- all of which have been addressed by the health care industry using one method or another.
 But there currently is only one strategy to prevent men from causing unwanted pregnancies; blocking the meeting of sperm and egg. This goal can take the several forms; reversible or irreversible barrier methods. The condom (left) is a reversible barrier method used by men to prevent pregnancy as well as transmission of sexually transmitted infections (STIs) such as genital warts, genital herpes and chlamydia. Unfortunately, due to improper or inconsistent use, the condom is not 100 percent effective. Further, many men complain that condoms decrease their sexual pleasure.
But there currently is only one strategy to prevent men from causing unwanted pregnancies; blocking the meeting of sperm and egg. This goal can take the several forms; reversible or irreversible barrier methods. The condom (left) is a reversible barrier method used by men to prevent pregnancy as well as transmission of sexually transmitted infections (STIs) such as genital warts, genital herpes and chlamydia. Unfortunately, due to improper or inconsistent use, the condom is not 100 percent effective. Further, many men complain that condoms decrease their sexual pleasure.
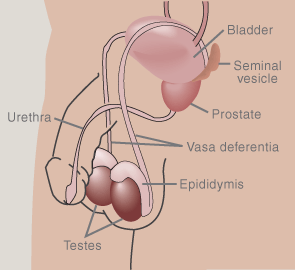 Unlike condoms, a vasectomy is a barrier method that is intended to be irreversible. It is a surgical procedure that causes sterility by blocking sperm from moving through the vas deferens from the testis and into the seminal fluid, thereby preventing pregnancy (see diagram, right). Even though they are permanent, vasectomies are nearly 100 percent effective and safe, and don't limit sexual pleasure.
Unlike condoms, a vasectomy is a barrier method that is intended to be irreversible. It is a surgical procedure that causes sterility by blocking sperm from moving through the vas deferens from the testis and into the seminal fluid, thereby preventing pregnancy (see diagram, right). Even though they are permanent, vasectomies are nearly 100 percent effective and safe, and don't limit sexual pleasure.
But scientists are developing another reversible contraceptive strategy for men: disrupting or stopping the proper development or maturation of sperm so they are either immobile or inviable or otherwise unable to fertilize an egg. To do this, researchers are investigating several methods. First and most obvious is the use of steroid hormones that prevent sperm from maturing properly, or second, the use of other drugs that damage sperms' ability to fuse with the egg.
Like female contraceptives, which rely on so-called "female" steroid hormones, the estrogens, along with the progestins to stop the release of eggs, male hormonal contraceptives rely on progestins and the so-called "male" steroid hormones, the androgens, to turn off sperm production. Another way to accomplish this same goal is to use androgens in conjunction with one of several drugs that block the action of Gonadotropin Releasing Hormone (GnRH). GnRH is a small protein hormone that triggers the release of the sex steroids; estrogens and androgens.
Unfortunately, altering a man's plasma testosterone levels can have undesirable side effects. Because testosterone contributes to sex drive, facial hair growth, bone and muscle mass maintenance, along with other physiological and behavioral effects, lower levels may result in fatigue, loss of muscle or decreased libido. So researchers found that pairing testosterone with Desogestrel, a synthetic progestin-like hormone that is the main component in many modern female contraceptive pills, resulted in normal hormone levels in the consequent clinical trials and thus, fewer side effects.
A hormone-based male contraceptive will likely be approved for use as either an implant (similar to Norplant, which is placed under the skin every 12 months), an injection that is given every three months, a patch that is applied directly to the skin or a gel that is embedded under the skin, or possibly as an oral contraceptive that is taken daily. At least one of these delivery methods is likely to be available in the United States in 5-7 years: implants and injections are currently undergoing clinical trials in China and plans are underway to begin Phase III trials in the USA within two years. However, whether there will ever be an oral contraceptive pill for men is more uncertain.
Interestingly, there are several other non-hormonal methods that have reversible contraceptive effects in men, too. For example, one such method is the medication Nifedipine, which is used to treat angina and to improve circulation. Nifedipine is a calcium channel blocker that relaxes the smooth muscles in arterial walls, reducing blood pressure. However, this drug also alters the structure of the cell membrane of sperm and thus blocks their ability to bind to an egg, preventing fertilization. The sterility effect usually wears off in 3 months, there are few side effects and Nifedipine does not appear to reduce the libido.
Several other drugs that have been used to treat hypertension or schizophrenia have also demonstrated contraceptive effects in men.
Another method that is currently under investigation involves tricking a man's immune system to destroy his own sperm. This relies on a protein produced in the testes and epididymis, called eppin, which facilitates sperm maturation. Basically, immunizing a man against eppin triggers an immune response in his body that results in reversible infertility.
So to summarize, the biological aspects of developing a safe, effective and reversible male contraceptive are more complicated than simply decrying this situation as being solely the result of sexual politics.
Sources
HowStuffWorks (see diagram).
- Log in to post comments

Thanks for addressing this and shedding light as to why it isn't necessarily a big pharma chauvinisitic conspiracy.
I'd heard something recently about men regularly taking very hot baths reducing their fertility. Supposedly there is even special designed underwear that warms the testis. I'm to understand sperm need a real goldilocks temperature to be viable. Does anyone know more about this method, and if it's reliable?
Men don't need a birth control pill because men don't get pregnant. Duh!
no, men don't get pregnant, but they do get slapped with multi-million dollar paternity suites.
I think that if I am a woman who wants birth control I am not going to trust that my partner is in charge of that. If a guy is concerned about paternity suits, than he might be interested but as far as women having a reliable method, I would not be willing to count on that.
Knowing how ridiculously suspicious men are of anything that they perceive as affecting their virility, I can't see this being a big seller.
JMHO
Men can also have wages garnished (unlawfully, BTW) in three states for child support that has already been paid, just ask my brother-in-law.
One major point is that women are fertile only part of the time, so it is easy to stall the cycle at an infertile point. No such cycle exists in men, so any cessation of spermatogenesis is unnatural.
Many years ago, (mid seventies) I read about 5-thio-D-glucose as a male birth control pill. Apparently is shuts down sperm production without the hormonal side effects. Does anybody know what happened with that?
great post!
bookmarked @ http://livbit.com
This is ridiculous. First, if you guys complain about a condom saying " It reduces pleasure...", someone should punch you in your dumb face because your a lazy lying sack of shit. Second, women....JUST TAKE THE PILL and stop bitching. Whats so hard about PUTTING ON A CONDOM and TAKING the DAMNED PILL?! Put away that bullshit feminist behavior and guys....don't be a lazy dumb shit and put the fucking condom on because I don't need your dumb ass kids to grow up making more posts and shit like this.
The only thing I'm ashamed of is that I had to use profanity to get the seriousness across and that I wasted my time writing to idiots. No I didn't read this post(good thing too or I would be more like the idiots that thought this)because the title and comments say it all.
bryan, you excellent anecdotal evidence in support for my argument that testosterone poisoning severely damages higher brain functions.
I'd heard something recently about men regularly taking very hot baths reducing their fertility.
The fertility prof at my alma mater liked to say that the only 100% effective method of birth control was two hours in a jacuzzi each day. It just does wonders for killing off sperm.
(When asked about abstinence, he'd say "My wife and I tried that, it didn't work")
no, men don't get pregnant, but they do get slapped with multi-million dollar paternity suites.
That's why men should have abortion rights. A male birth control pill is just a medical attempt to solve a legal problem.
Thanks GrrlScientist, you proved to MY argument that women just can't stop being a feminist and always have to get the last word in. Oh, and before you use words like anecdotal(you still get 10 points for correct use so don't cry), try spelling a little better. Maybe use some caps for the start of a sentence and names. For a GrrlScientist, you sure don't live up to the name. I figured with all that schooling you'd know that. What a waste of your money.
Now if you read my prior comment correctly(if you can read correctly), you would see that I'm not picking on just women. Men are being idiots as well. Now with that said just let it go, accept it, and move on with you life to things that actually matter.
You do know that hormonal birth control pills fuck up some women, right? Putting a big slug of estrogen into yourself every day works OK for some, but not for others -- and a birth control method that makes you not want to have sex is just a horribly dumb thing. The depression isn't so great either.
Bryan: why comment so vehemently on a post that was written to answer a question? It's as though GrrlScientist arranged for a plant in the audience to ask such an obviously controversial question, for no other reason than to enrage you. Although I agree that both men and women complain unduly regarding the actual administering of birth control, that doesn't nullify the discussion of possible methods. In any case, cursing is not necessary in order for one to get one's point across (even forcefully), and in fact is indicative of a probable linguistic impotence.
I personally thought the post was informative and rather interesting (thanks, GrrlS, for your educated opinion), as I've never really thought about the issue myself. It certainly has always seemed to me that controlling the hormonal estrus cycle of women was chemically simpler than trying to "turn off" a constant production in men. The fact that there are highly effective, reasonably inexpensive and even non-hormonal birth control methods available to women is indicative of our society's scientific progress.