![]() After a lot of the not-so-Respectful Insolence⢠of the last couple of weeks, I've been meaning to get back to living up to the name of the overall mega-blog, namely ScienceBlogs. Meeting up with my fellow SB'ers over the weekend in New York Fortunately, last week a topic just so happened to pop up related to my area of expertise, when a study in The Lancet was published evaluating the use of MRI in breast cancer. It happened to get a bit of press when it came out last month, some of it a bit breathless, as though this were a revolutionary observation. (To some extent it was unexpected, but it wasn't really revolutionary.) I'm also waiting with a little bit of trepidation for my patients to start asking about it or to start demanding MRI once again, as I did a few months ago when some rather poorly justified guidelines were published by the American College of Physicians. Don't worry, though. I'm sure I'll find some red meat topics again soon enough.
After a lot of the not-so-Respectful Insolence⢠of the last couple of weeks, I've been meaning to get back to living up to the name of the overall mega-blog, namely ScienceBlogs. Meeting up with my fellow SB'ers over the weekend in New York Fortunately, last week a topic just so happened to pop up related to my area of expertise, when a study in The Lancet was published evaluating the use of MRI in breast cancer. It happened to get a bit of press when it came out last month, some of it a bit breathless, as though this were a revolutionary observation. (To some extent it was unexpected, but it wasn't really revolutionary.) I'm also waiting with a little bit of trepidation for my patients to start asking about it or to start demanding MRI once again, as I did a few months ago when some rather poorly justified guidelines were published by the American College of Physicians. Don't worry, though. I'm sure I'll find some red meat topics again soon enough.
Here's the press release from the University of Bonn, Germany, where the study was done:
A study in the Lancet (vol. 370, 11 August 2007) could lead to a change of paradigm in the early diagnosis of breast cancer. It states that magnetic resonance imaging (MRI) is substantially more accurate than mammography in diagnosing very early stages of breast cancer . Up to now MRI was thought to be hardly suited for the detection of such 'ductal carcinoma in situ (DCIS) . Researchers at the University of Bonn have now come to a completely different conclusion. In the past five years they examined more than 7000 women with both methods. In a total of 167 women the doctors found early forms of breast cancer - 152 (92 %) of these were found using MRT, 93 (56 %) with mammography.'
This sounds pretty awesome, doesn't it? With MRI, they appear to be picking up nearly twice as much DCIS. This has to be a good thing, right? Well, as I explained before, maybe yes, maybe no. Before I go on, I'll explain a bit what DCIS is. It's a bit of a strange beast in a way. I generally characterize it to my patients as breast cancer that has not yet broken out of the milk ducts to invade the surrounding tissue. We call it "carcinoma," although it's variable in its clinical behavior and it is controversial whether it always represents a precursor to full-blown invasive breast cancer. In other words, this is one of those diseases where it's not always clear whether or not it will ever progress to threaten a woman's life. Our best understanding of breast cancer thus far suggests that almost all breast cancer starts out at DCIS, but we don't know what percentage of DCIS ever progresses to frank breast cancer that can threaten a women's life. Some of it may be quite indolent, while some of it may progress with a high probability to cancer. One thing we do know is that local therapy with surgical excision and radiation therapy can cure DCIS quite reliably. Because we can't predict which case of DCIS will be a bad actor, we therefore treat it all pretty much the same way in order to prevent its progression.
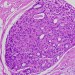
Fortunately, we're not totally without guidance in deciding which cases of DCIS are likely to be dangerous and which are not. DCIS, like all breast cancer, is divided up into "grades," based on how much their nuclei look like normal nuclei. Low grade tumors have nuclei that look pretty close to the same as normal breast epithelia. High grade tumors, on the other hand, have bizarre-looking nuclei that look very abnormal, and pathologists have set up criteria to differentiate low form intermediate from high grade tumors. High grade tumors, not surprisingly, appear to progress to invasive breast cancer much more reliably than low grade tumors, which may not progress at all. Indeed, we use this criteria sometimes in deciding whether to do radiation therapy after surgery or to give estrogen-blocking drugs to prevent recurrence.
So let's get to the study. Here's the abstract:
Christiane K Kuhl, Simone Schrading, Heribert B Bieling, Eva Wardelmann, Claudia C Leutner, Roy Koenig, Walther Kuhn, Hans H Schild. MRI for diagnosis of pure ductal carcinoma in situ: a prospective observational study. Lancet 2007; 370: 485-92.
Background: Diagnosing breast cancer in its intraductal stage might be helpful to prevent the development of invasive cancer. Our aim was to investigate the sensitivity with which ductal carcinoma in situ (DCIS) is diagnosed by mammography and by breast MRI.
Methods: During a 5-year period, 7319 women who were referred to an academic national breast centre received MRI in addition to mammography for diagnostic assessment and screening. Mammograms and breast MRI studies were assessed independently by diff erent radiologists. We investigated the sensitivity of each method of detection and compared the biological profiles of mammography-diagnosed DCIS versus DCIS detected by MRI alone. We also compared the risk profi les of women with mammography-detected DCIS with those of MRI-detected DCIS.
Findings: 193 women received a final surgical pathology diagnosis of pure DCIS. Of those, 167 had undergone both imaging tests preoperatively. 93 (56%) of these cases were diagnosed by mammography and 153 (92%) by MRI (p<0·0001). Of the 89 high-grade DCIS, 43 (48%) were missed by mammography, but diagnosed by MRI alone; all 43 cases missed by mammography were detected by MRI. By contrast, MRI detected 87 (98%) of these lesions; the two cases missed by MRI were detected by mammography. Age, menopausal status, personal or family history of breast cancer or of benign breast disease, and breast density of women with MRI-only diagnosed DCIS did not differ significantly from those of women with mammography-diagnosed DCIS.
Interpretation: MRI could help improve the ability to diagnose DCIS, especially DCIS with high nuclear grade.
Although this is not a double-blind randomized study, it is a solid design to take an initial look at the research question examined, namely the sensitivity of MRI in diagnosing DCIS. For on thing, it's a prospective, not a retrospective study, which means that the investigators looked at cases from the very beginning according to a preplanned study design, with criteria for evaluating the data decided upon before the first patient was ever enrolled. This is generally a better design than retrospective studies, where preexisting patient data is analyzed, meaning that standardization can be a problem. But, worse, the very fact that such studies require deciding upon criteria for analysis after the data has already been detected makes them much more prone to bias or effects from confounding variables that aren't always obvious. In the case of this study, women generally underwent mammography for one of four reasons:
- A non-normal screening mammogram.
- Normal conventional imaging studies, but clinical symptoms of breast cancer.
- Normal conventional imaging studies, but at an increased risk for (primary or recurrent) breast cancer.
- Normal conventional imaging and an average risk, but were concerned about breast cancer and wished to undergo MRI as an additional screening test.
The investigators also looked at the interpretations of the mammograms and MRIs independent of each other and of the pathologic diagnosis from biopsy, so that none of the results could influence each other. Of course, this is somewhat artificial, because most MRIs are presently ordered on the basis of an abnormal mammogram or an equivocal abnormality on physical exam plus normal mammography and ultrasound. However, it does allow evaluation of the sensitivity and specificity of MRI as a single test, although, as the authors conced, the knowledge of the four criteria listed above for MRI could have subtly biased the radiologists interpreting the MRIs. This is the same bias present in the old studies of MRI, namely knowledge of the fact that MRIs are generally ordered only when there is a physical finding or a mammographic abnormality.
The question of whether MRI is as good as or better than mammography in detecting DCIS is of considerable interest because most studies to date have suggested that, although MRI is definitely more sensitive for breast cancer, it may not be as good as mammography for detecting DCIS. The reason was thought to be that most DCIS is detected on mammography by the presence of microcalcifications, tiny calcium deposits that are often found there and that are thought to be due to dying cells. MRI doesn't detect microcalcifications. Rather, it detects differences in patterns of blood flow, and it was thought that the differences in such patterns, which are striking in invasive cancer, were more subtle and difficult to detect in DCIS.
The most striking and potentially interesting result here is the distribution of DCIS found by the two different imaging modalities. MRI detected the high grade lesions far more effectively than mammography did, while mammography tended to detect the lower grade lesions, which are less likely to be dangerous. This is different than what was expected, although it is biologically plausible. After all, high grade lesions are "closer" to cancer and would be expected to have more blood vessels and more blood flow.
In light of a study like this, then, should we be ordering MRIs for every woman? I'm not yet convinced, for reasons that I discussed in detail before. Once again, because of the phenomena of lead time bias, length bias, and stage migration, the increased sensitivity of MRI for DCIS may or may not lead to a decrease in mortality with wider usage. That determination will await studies designed to look at just that question, and, although the authors of the study were appropriately circumspect in the article itself, one of them, Professor Kuhl, isn't quite so circumspect in the press release, when she claims that her study "demolishes a number of textbook dogmas." Not exactly. Given how new MRI is and how fluid the research on its role in breast cancer is, I'd be hard-pressed to say that any belief about it has had time to harden into "textbook dogma." This was just a minor irritant, though. No doubt Professor Kuhl felt the need to sell the results of the study for the press release, even though the article pretty much sells itself to anyone involved in breast cancer.
There is one huge problem with this study. It's not the methodology, which was sound, but rather how to apply its results to the general population. MRI, although becoming more widely available, is still difficult to come by outside of large urban centers. Moreover, there is as yet nowhere near the capacity, as far as MRI facilities and trained radiologists to interpret the MRIs, to use it as a mass screening tool, leaving aside the fact that it has not yet been shown that the use of MRI results in an actual decrease in mortality due to breast cancer among women. Also, the researchers at Bonn used a new, specialized protocol to detect DCIS. The majority of radiologists who do interpret breast MRI now are probably unfamiliar with it. Consequently, although this study suggests to me that I should probably be less reluctant to embrace MRI wholeheartedly (and, indeed, I've noticed that I seem to be ordering more MRIs these days), we still have a lot of work to do to clarify the role of MRI.


Thanks for this.
MRI has serious advantage over mammography. MRI's are as far as I know not detrimental like X-ray which is used in mammography. I'm not dead certain about this so please correct me if I'm wrong. Also while mammography detects the tumor it's hard to precisely pinpoint the location. MRI, combined with MRA would be able to locate the tumor and map the blood flow to it in 3-D. MRIs are great at mapping changes in tissue densities. The varied densities was what I though allowed one to feel the lump. X-ray CT can map the body in 3-D but but requires quite a lot more radiation and I don't know of any tomographic mammography.
I would think this would make it easier to kill the tumor with much less damage to surrounding tissue. I know next to nothing about the procedures used to kill the tumors surgically, beyond that they are removed.
As far as anyone knows right now, MRI is indeed safer than x-ray, because it doesn't involve any ionizing radiation. It has two main drawbacks: 1) it's rather intimidating for the claustrophic, and 2) it's a heck of a lot more expensive.
Part of the reason that an MRI is so expensive is that they are built much the same way as a top end road rocket. Built to order. If there was a call for more MRI systems the build cost would go down. Also if there were more MRIs and more frequently used there would be a call for requiring MRI skills for graduating from Med school. Thus creating more MRI techs and lowering the cost of staffing. The cost of powering these things will still keep going up though.
The claustrophobia can at least be mitigated with open MRI. However I don't know the imaging limitations of open vs closed MRI. I don't know if open MRI can image with the same resolution.
I recall reading somewhere that it may be possible to build smaller MRI units for use in mammography and imaging of extremities, and that such units may be able to use conventional magnet coils (i.e. not cryogenic superconductors). If this turns out to be true then the cost could be driven down substantially. These units are more likely to be portable too, which could improve non-urban access.
Open MRI magnets are much weaker than closed MRIs. Open MRIs are typically .3 tesla while most closed MRI nowdays are 1.5 tesla -- there are stronger magnets but 3 tesla machines are rare still.
Extremity MRIs already exist, so redesign of these models to suit breast scanning shouldn't be too hard.
There are some side-effects with getting an MRI scan. It's rare, and most people won't experience anything, but it happens. Long term effects are not yet known, it hasn't been around long enough to know what'll happen to those folks on 3 month scan schedule. So... it might not be as safe as people think it to be. I always get hot during a scan... Start off freezing cold and by the end I'm sweating.
One advantage I see for MRI is with women like myself who have breast implants. My implants are 17 years old and I'm concerned that a mammogram might cause a rupture, so I've avoided mammograms for a few years. I'm thinking about asking my ob/gyn about getting an MRI instead.
You forgot another huge drawback of MRI. Breast MRI requires an injection of intravenous gadolinium contrast, something I forgot to mention. Although serious reactions are uncommon, they occur at a rate as high as 0.01%. Even though that's an estimate of the high end, if we start doing a lot more MRIs for breast, either for screening or diagnosis, you can expect that the number of life-threatening reactions to gadolinium will dramatically increase. If you do 1,000,000 breast MRIs, it's possible that as many as 100 women might have severe reactions, although probably the number will be considerably lower. Even so, do enough MRIs, and there likely will eventually be a handful of deaths. The same can't be said of mammography.
Very well written and balanced exposition, and several of the comments are interesting as well. Thanks much.
One slightly off the wall question that occurred to me as I read this post was whether anyone reading this has looked at thermography--either as an addition to or substitute for MRI and/or mammography. Don't know much about it, but have seen it mentioned in somewhat positive light. Anyone know anything about it?
If we were talking about cancer on your testiticles, I bet you wouldn't mind paying for an expensive MRI? Right?
I bet if we were talking about testicle cancer on your bottom, an MRI wouldn't appear to be too expensive? Right?